Uniportal lobectomy in Africa: a beginning
Introduction
Thorascopic lobectomies have been performed in Southern Africa since the early 1990’s (1). This is an ongoing area of surgery that although being available for at least 20 years worldwide has not become the universal approach. Most lobectomies are still performed with a full thoracotomy. The reasons are surgeon’s preference, large tumors presenting later than stage 1, their training, the limited experience with thorascopic techniques and inability to visualize in a 2-D environment. These factors all influence surgeon’s preference. Uniportal lobectomy is an attempt to combine the advantage of video assisted thoracic surgery (VATS) and open surgery.
Patient selection and workup
During August 2015 an animal wet-lab was arranged to demonstrate the techniques in South Africa. The visiting expert was Prof. Gonzalez-Rivas from Coruna Spain. Following the wet-lab Prof. Gonzalez-Rivas visited four of the South African medical schools demonstrating his techniques. The cases chosen were stage 1 tumors, benign conditions as well as mediastinal masses in which a similar approach to a lobectomy could be demonstrated. The work also emphasized the importance of screening for lung cancer in a group of patients with a high incidence of lung cancer. The patients were chosen by the academic centers but Prof. Gonzalez-Rivas confirmed the suitability for surgery before the procedures were performed. The indications for surgery were the standard as for any thoracotomy. The work-up was no different. We did request stage 1 cancers if possible.
Equipment
Each center had different thorascopic camera systems. The only additional equipment was thorascopic instruments supplied by Scanlan, vascular clips supplied by Grena and Endo-Gia staplers supplied by Covidien (Medtronic).
Procedure
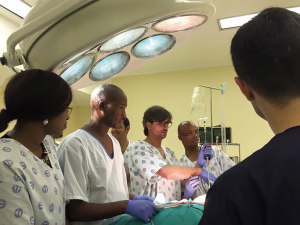
The patients (Figure 1) were placed in a full lateral position with a support under the patient. The surgeon and assistant operated from the front of the patient allowing access to the vascular structures first. A 30-degree scope was utilized.

The standard indications are as for any thoracic procedure. VATS is performed for diagnostic as well as therapeutic procedures. In my practice it has replaced an anterior mediastinotomy (Chamberlain procedure) as a far less invasive but also superior procedure that allows far greater visualization of the pleural cavity, the entire mediastinum allowing the surgeon to perform biopsies safely with greater accuracy than the standard operation.
Post-operative management
Patients were mobilized as soon as they were awake from the anesthetic. Patient kept as pain free as possible. During the tour the individual hospitals did the post-operative care and discharge of the patients. No complications were experienced.
Discussion
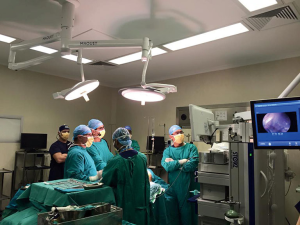
South Africa is an emerging economy with a constant emphasis on saving money. At the same time we pride ourselves on the standard of our healthcare facilities. We have centers of excellence that match the standard of the best in the world. At the same time however our training in modern techniques has suffered due to the lack of modern equipment. This program of uniportal VATS with the wet lab (Figure 2) as well as the visits to four medical schools was an attempt to introduce VATS as the standard of care in a modern tertiary care hospital.
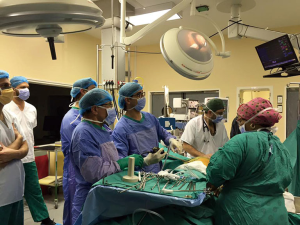
The program started with a wet lab utilizing pigs in which 27 young surgeons were exposed to VATS techniques. This was followed by visits to four medical schools. Starting at Tygerberg Hospital (Figure 3), we travelled to Durban (Albert Luthuli Hospital, University of KwaZuluNatal), University of Pretoria and finally the Sefako Makgatho University.
A uniportal VATS lobectomy was performed at each of the universities plus a variety of other VATS procedures. A VATS posterior mass was resected, a massive bullous was removed with preservation of the collapsed lung (Figure 4).
A striking feature of all four visits was the hunger to learn by the entire departments but in particular the young registrars and newly qualified surgeons.
VATS lobectomies can be performed as a uni-portal approach, a two-port, three-port and also in some centers a multiport approach. The very important point is that there is no spreading of ribs. The uni-portal approach is a combination of the open operation and a VATS approach. While the surgeons are learning the procedure the incision starts as a longer incision gradually becoming smaller and smaller until it is not more than 3 cm in length. It allows the surgeon to have the confidence to do the procedure knowing he can always open the chest. It is also a more intuitive approach, as the vision is more like what they are used to. Very important no spreading of the ribs is required even with removal of fairly large masses. It is my own experience not only in my patients but also in watching other surgeons that VATS surgeons are more careful in their dissection of the hilum as well as in the lymph node dissection including the sub-carinal space. Vision is magnified with a far better view of the structures. With the 30% thoracoscope the entire pleural cavity can be visualized. Thoracoscopy has stimulated the development of new instruments making the operations safer and much easier. This includes numerous instruments, staplers and clips. During the tour we utilized Scanlan instruments, Covidien and Ethicon staplers and Grena clips. The Scanlan instruments and Grena clips were designed by Prof. Gonzalez-Rivas and simplify the procedures.
Modern thorascopic surgery began in 1991. Lobectomies were performed in the early 1990’s through multiple ports. Uniportal VATS has developed over the last about 10 years (3).
The standard thoracic operating theatre in my opinion should always have thorascopic instruments available. Although we still need the ability to perform open surgery the standard should be VATS. Just as other branches of surgery have evolved, so has cardiothoracic surgery. The speciality is totally different to what it was 30 years ago and will continue to change (4-6).
Africa is going through a development that is faster than most of the rest of the world. The training of medicine and particularly surgery needs to mirror this development (7,8).
Results
Since Prof. Gonzalez-Rivas’s visit VATS programs have commenced at all four universities. Stellenbosch University will be performing their first VATS lobectomy in January 2016. As in all programs the programs have commenced with simple procedures such as lung biopsies, early pleural toilet and decortications before proceeding to the more advanced operations.
During 2016 thorascopic surgery will be introduced to Namibia and Botswana as well as a further tour of South Africa to visit the other medical schools and to encourage our local surgeons.
The opinion in this report is mine and is an appeal to African medical schools to maintain the very high standards that, in my case South Africa, has been justly proud of.
Acknowledgements
The program was supported financially by Covidien.
Footnote
Conflicts of Interest: The author has no conflicts of interest to declare.
References
- Schewitz I. Update on Thorascopic Surgery-Minimally Invasive Thoracic Surgery. S.A. Respiratory J 1996;13-6.
- Schewitz I. Roadshow in South Africa. Asvide 2016;3:107. Available online: http://www.asvide.com/articles/861
- Ng CS, Gonzalez-Rivas D, D'Amico TA, et al. Uniportal VATS-a new era in lung cancer surgery. J Thorac Dis 2015;7:1489-91. [PubMed]
- Gonzalez-Rivas D, Paradela M, Fernandez R, et al. Uniportal video-assisted thoracoscopic lobectomy: two years of experience. Ann Thorac Surg 2013;95:426-32. [Crossref] [PubMed]
- Aragón J, Pérez Méndez I. From open surgery to uniportal VATS: asturias experience. J Thorac Dis 2014;6:S644-9. [PubMed]
- Ismail M, Helmig M, Swierzy M, et al. Uniportal VATS: the first German experience. J Thorac Dis 2014;6:S650-5. [PubMed]
- Ng CS, Rocco G, Wong RH, et al. Uniportal and single-incision video-assisted thoracic surgery: the state of the art. Interact Cardiovasc Thorac Surg 2014;19:661-6. [Crossref] [PubMed]
- Gonzalez-Rivas D, Aymerich H, Bonome C, et al. From Open Operations to Nonintubated Uniportal Video-Assisted Thoracoscopic Lobectomy: Minimizing the Trauma to the Patient. Ann Thorac Surg 2015;100:2003-5. [Crossref] [PubMed]
Cite this article as: Schewitz I. Uniportal lobectomy in Africa: a beginning. J Vis Surg 2016;2:54.