Endovascular stent graft for surgical resection of lung cancer invading aortic arch: report of a 79-year-old patient
Introduction
The surgical indications for non-small cell lung cancer with aortic involvement are currently unclear. Some reports have described a relatively favorable prognosis of T4N0–1 disease when the invaded aortic wall is completely resected (1,2). Combined resection of the aorta and lung may require cardiopulmonary bypass (CPB) or extra-anatomical bypass, which are associated with high morbidity and mortality. Considering the invasiveness of this surgical intervention, relatively young patients without other complications are candidates for surgery whereas those with comorbidities or elderly patients are thought to be ineligible for resection. Aortic stenting followed by lung resection might be an alternative procedure for patients with lung cancer invading the thoracic aorta. Here we describe an elderly patient with chronic obstructive pulmonary disease who underwent en bloc resection of the lung and aortic arch following intra-aortic stent grafting.
Case presentation
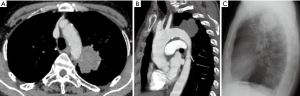
A 79-year-old man was referred to our hospital for evaluation of an abnormal chest shadow. He was an ex-smoker with chronic obstructive pulmonary disease. Forced expiratory volume in one second (FEV1) was 2,030 mL and FEV1% was 57%. Computed tomography (CT) showed an irregular-shaped mass of 6 cm diameter in the left upper segment, widely abutting the distal aortic arch (Figure 1A,B). Sputum cytology revealed squamous cell carcinoma. [18F]-fluoro-2-deoxy-D-glucose positron emission tomography (FDG-PET) showed increased uptake in the tumor with a maximum standardized uptake value of 23. No metastases to the hilar or mediastinal lymph nodes were seen. No other metastases were detected on chest CT, brain magnetic resonance imaging (MRI), or FDG-PET. Intravascular ultrasonography strongly suggested invasion of the lung cancer into the aortic wall. Considering the patient’s age and spirogram, concomitant resection of the aortic wall using CPB support was not indicated. Endovascular stenting prior to resection to enable en bloc resection of the lung and aortic wall without CPB support was performed. A thoracic endovascular graft (Relay; Bolton Medical, Barcelona, Spain) with a proximal bare stent (34-mm proximal and 30-mm distal diameter; 162-mm length) was placed from the distal arch to the descending aorta under general anesthesia. The landing zone was 25 mm proximal to the left subclavian artery, and the covered portion of the stent was adjusted distal to the left subclavian artery (Figure 1C). No procedure-related complications occurred, such as stroke, paraplegia, or leakage. The patient underwent left upper segmentectomy with aortic medial decortication by a lateral thoracotomy through the fifth intercostal space 20 days after the aortic stenting. Decortication of the aortic adventitia and some medial layers was easy and safe with support from an intra-aortic stent (Figure 2). The total operation time was 176 min. The intraoperative blood loss volume was 350 mL and no blood transfusion was necessary. The removed specimen included a 3-cm × 4-cm flap of aortic wall, and the defect was not buttressed. Pathologic examination revealed a T4N0M0 squamous cell carcinoma with infiltration into the aortic adventitia. No cancer remained on the surgical margin. The patient postoperative course was uneventful other than paroxysmal atrial fibrillation, which improved with medication. The patient was discharged on postoperative day 18. He returned to daily life without any graft-related complications or any recurrences 2.5 years after surgery. The FEV1 and FEV1% had improved to 2,130 mL and 72%, respectively, 1 year after surgery.

Discussion
When combined aortic and pulmonary resection is performed in patients with locally advanced lung cancer, patch plasty or sleeve resection with reconstruction by a graft is usually required. CPB or temporary extra-anatomical aortic bypass is generally recommended to prevent organ ischemia. Because this procedure is accompanied by high morbidity and mortality associated with organ ischemia and/or embolic events, surgical candidates are carefully selected, and elderly patients or those with comorbidities should not be eligible. Thoracic endovascular aortic stent grafting followed by combined resection of the aorta has been reported as a novel method for patients with thoracic malignant tumors invading the aorta (4-7). The most beneficial aspect of this procedure is that concomitant resection of the aortic wall can be performed without CPB. All patients who have undergone this less invasive manipulation were younger than 70 years old (4-7). Aortic stent grafting for combined resection of the aorta may be feasible in elderly patients with high-risk patients.
Aortic invasion is mostly limited within the adventitia when lung cancer is diagnosed as operable (8). Therefore, combined aortic resection can usually provide a sufficient surgical margin when aortic resection includes some medial layers. Supplementary Figure 2 shows that prior endovascular stenting allows the easy identification of the medial layer during aortic decortication.
The optimal duration between intra-aortic stent placement and aortic decortication is unclear; in previous reports, this duration ranged from 1 to 17 days (4-7). This time interval can cause stent-related complications that might not occur if stent grafting and lung cancer resection are performed during a one-stage procedure.
Some problems may be associated with stent graft placement for lung cancer invading the aortic arch. The decision making of aortic stent grafting is the first issue. Cine dynamic MRI is a useful diagnostic tool for aortic invasion of lung cancer. However, the evaluation of major structures with minimal-to-no motion such as the distal aortic arch is limited on cine MRI (9). Therefore, a definite diagnosis should be made via exploratory thoracoscopy or thoracotomy, when intravascular ultrasonography cannot identify aortic invasion, as in our case. Second, the aortic arch is a challenging site for endovascular stenting, because of its branching pattern. When the stent graft is placed in the aortic arch, the use of a fenestrated stent graft or crossover bypass from the right-to-left common carotid artery reportedly helped to maintain the blood flow to the arch branches (6,7). The Relay graft with a proximal bare stent is useful because it is highly efficient in patients with an angulated aortic anatomy and is associated with a low incidence of endoleakage (10). Moreover, its stability is satisfactory when a large landing zone of the proximal bare portion of the stent can be sufficiently secured while the blood flow into the arch branches is preserved. Although aortic wall defects were reinforced using a latissimus dorsi muscle flap and Hemashield fabric patch (MAQUET, Rastatt, Germany) in previous reports (6,7), the device was sufficiently thick and firm for the arterial defect.
In conclusion, the combined resection of the aortic arch and left upper segment following endovascular stent for advanced lung cancer in a 79-year-old man with pulmonary compromise was successful. Innovated endovascular stenting is an alternative to radical surgery for locally advanced lung cancer.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The study was approved by the ethnical committee. Written informed consent was obtained from the patient. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
References
- Ohta M, Hirabayasi H, Shiono H, et al. Surgical resection for lung cancer with infiltration of the thoracic aorta. J Thorac Cardiovasc Surg 2005;129:804-8. [PubMed]
- Chambers A, Routledge T, Billè A, et al. Does surgery have a role in T4N0 and T4N1 lung cancer? Interact Cardiovasc Thorac Surg 2010;11:473-9. [PubMed]
- Otani S, Tsubochi H, Endo S, et al. An aortic decortication of the distant aortic arch following left upper segmentectomy for the advanced lung cancer. Asvide 2016;3:040. Available online: http://www.asvide.com/articles/791
- Marulli G, Lepidi S, Frigatti P, et al. Thoracic aorta endograft as an adjunct to resection of a locally invasive tumor: a new indication to endograft. J Vasc Surg 2008;47:868-70. [PubMed]
- Berna P, Bagan P, De Dominicis F, et al. Aortic endostent followed by extended pneumonectomy for T4 lung cancer. Ann Thorac Surg 2011;91:591-3. [PubMed]
- Nagata T, Nakamura Y, Yamamoto H, et al. A fenestrated stent graft for surgical resection of lung cancer invading the aortic arch. J Thorac Cardiovasc Surg 2013;146:238-9. [PubMed]
- Collaud S, Waddell TK, Yasufuku K, et al. Thoracic aortic endografting facilitates the resection of tumors infiltrating the aorta. J Thorac Cardiovasc Surg 2014;147:1178-82; discussion 1182. [PubMed]
- Misthos P, Papagiannakis G, Kokotsakis J, et al. Surgical management of lung cancer invading the aorta or the superior vena cava. Lung Cancer 2007;56:223-7. [PubMed]
- Seo JS, Kim YJ, Choi BW, et al. Usefulness of magnetic resonance imaging for evaluation of cardiovascular invasion: evaluation of sliding motion between thoracic mass and adjacent structures on cine MR images. J Magn Reson Imaging 2005;22:234-41. [PubMed]
- Riambau V, Zipfel B, Coppi G, et al. Final operative and midterm results of the European experience in the RELAY Endovascular Registry for Thoracic Disease (RESTORE) study. J Vasc Surg 2011;53:565-73. [PubMed]
Cite this article as: Otani S, Tsubochi H, Endo S, Yuri K. Endovascular stent graft for surgical resection of lung cancer invading aortic arch: report of a 79-year-old patient. J Vis Surg 2016;2:20.


