Uniportal video-assisted thoracoscopic lobectomy: Zhongshan experience
Historical note
Uniportal video-assisted thoracoscopic (VATS) is an emerging technique in the field of thoracic surgery. Since the first report on uniportal thoracic surgery by Rocco in 2004, the topics on pneumothorax, pleural biopsy, and lung wedge resection using uniportal VATS have shown promising results (1). In 2011, Gonzalez et al. reported their experience on thoracoscopic lobectomy through single port, which was the first published study on major lung resection (2,3). Following that were the manuscripts on complicated cases using uniportal sleeve or even double-sleeve lobectomy within very short periods of time (4). The emerging technique, as an ever-progressive procedure, further pushed the advancement of thoracic surgery (5,6).
Up to date, with growing evidence on feasibility and safety, uniportal VATS was world-widely welcomed. In a recent report from Dr. Venuta, uniportal VATS was even well practiced by hands without VATS experience (7). Meanwhile, there remained a large number of medical centers in which uniportal VATS lobectomy was never ever practiced, due to technical difficulties. In this chapter, we aimed to describe uniportal VATS lobectomy that was conventionally performed in an Eastern center, which might help facilitate a good beginning in practice this technique.
Indications
The indications of uniportal VATS lobectomy are merely equal, if not the same, to multiportal VATS lobectomy. The benign indications for lobectomy include carcinoid tumors, fungal and bacterial infections, chronic bronchiectasis, tuberculosis infection of the lung, and congenital malformations. In the cases of malignancy, pre-operative examination including electrocardiogram (EKG), pulmonary function, chest computed tomography (CT) scan, bronchoscope, and brain magnetic resonance imaging (MRI) would be administered to exclude the candidates for curative surgery. The stage III patients in together with some surgically resectable patients would be included in uniportal VATS lobectomy.
Anesthesia and analgesia
All patients would receive a combination of epidural and general anesthesia, and were provided with patient-controlled analgesia (PCA) postoperatively. After intravenous induction, each patient was intubated with a double-lumen endotracheal tube to accomplish single lung ventilation. All patients were extubated at the end of surgery and transferred to the ward. Local anesthesia to the incision using 0.2% bupivacaine is recommended during the wound closure.
Positioning
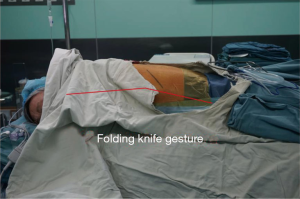
Generally, the patient was kept in a folding knife gesture (with the cranial side slightly raised up and caudal side pushed down) in lateral decubitus position (Figure 1). Intra-operatively, the surgeon and the assistant stand on the abdominal side of the patient. The assistant stood at the foot-stool. The entire procedure was performed under the screen observation.
Incision
In uniportal VATS lobectomy, the surgical resection around hilar would be the major part to the whole procedure. Since there would be only one port available, the optimal distance between hilar and the port would facilitate the lobectomy. Besides, the limited width of the incision would interfere the surgical instruments when passing through the incision, and the hilar as well, which required an additional angel between the incision and the hilar. So the role of incision positioning should take both the distance and angle into the consideration. Due to the anatomic variation, the hilar would be positioned close to the level of 4th-5th intercostal space. It would be helpful to locate the hilar according to CT scan before operation. Conventionally, an incision (th intercostal space (Figure 2) for upper lobe resection and 5th intercostal space for middle and inferior lobe resection.
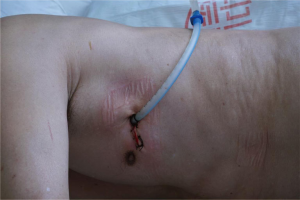
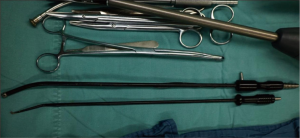
A soft plastic wound protector was applied to the incision without rib-spreading procedure. The protector minimized iatrogenic touch during the introduction of thoracoscope to the surgical field, especially in the cases of obesity patients with thick subcutaneous fat tissues. A 10-mm 30 degree thoracoscope would be positioned in the superior side of the incision during the whole procedure. The designed surgical instruments (Figure 3), in together with the harmonic shear (Ethicon Endo-Surgery Inc, Cincinnati, OH, USA) or hook electro-cautery were applied during the procedure.
Thoracic exploration
In uniportal VATS lobectomy, the geographical view differed from multiportal VATS, while the thoracic cavity required carefully exploration to identify any unexpected invasion or metastasis. Since the incision was located at the anterior axillary line close to the anterior part of the hilar, the posterior part of the hilar, and diaphragm were far from the surgical incision. Therefore the identification of incidental lesion at these locations remained important before the confirmation of the lobe resectability.
Management of the hilar vessels
The procedure continued from the diaphragm exploration to the taken down of the inferior pulmonary ligament. Usually, care must be taken not to injure the inferior pulmonary vein. The lobectomy around hilar included the identification and dissection of the three primary vascular structures: the pulmonary artery, the superior pulmonary vein, and the inferior pulmonary vein. Venous drainage of each lobe is confirmed, and any anatomic anomalies are identified. The order of dissection and transection differed in upper and lower lobectomy (detailed below). Cautery can be used on the posterior aspect of the hilum, but care must be taken anteriorly to avoid thermal injury to the phrenic nerve.
Management of the fissure
In uniportal VATS, a complete or incomplete makes the difference between a very simple resection and a tedious and difficult one. Similar to the multiportal VATS, complete fissures allowed identification of the pulmonary artery as a landmark to begin dissection. Otherwise, the fissureless technique would be considered to deal with the fissure as the last step during the surgical resection of the target lobe. In dissecting the fissure, make sure that the staple line covered both surfaces of the lung and no remaining parenchymal is left after the fire of the staple. Besides, an uncertain staple line might be tested for air leak and oversaw strengthen.
Upper lobectomy
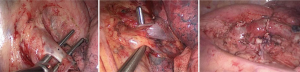
Previously, upper lobectomy using VATS technique was considered more difficult in compared with lower lobectomy. The dissection of truncus anterior branch of pulmonary artery remained as the challenging part during the upper lobectomy. Besides, if the surgery started from the dissection of major fissure, which was not always well developed, would increase the difficulty towards lobectomy. On the contrary, in uniportal VATS upper lobectomy, the surgery usually started from the dissection around the hilar, and truncus anterior artery was usually kept as the first main vessel to be dealt with. The dissection order was modified to facilitate the whole procedure. After the dissection of truncus anterior artery, the upper bronchus would be exposed, and the dissection would be easy. The artery, bronchus, and vein were divided and dissected separately using an endo-linear stapler (Covidien, Mansfield, MA, USA or Ethicon Endo-Surgery Inc, Cincinnati, OH, USA) (Figures 4,5) (8).

Lower lobectomy
In the cases of lower lobe lesions, the dissection order varied according to the development of the major fissure. When the oblique fissure developed well, the basal and the posterior branch could be mobilized easily. The procedure would be followed by dissection of the lower bronchus and then the inferior pulmonary vein. Since the incision was located at the 5th intercostal space, which was close to the major fissure, the dissection along the fissure was facilitated without turning over the lower lobe.
When developed fissure was not observed or the lesion was close to the fissure, it would be easier to start the dissection from the inferior ligament. The inferior pulmonary vein was switched to the first main vessel during the whole procedure. The procedure was similar to the “single direction lung resection” described by Dr. Lunxu Liu and associates (9). In that case, the surgeon and assistant would change their positions to facilitate the dissection along the inferior ligament.
Middle lobectomy
Usually, a lesion located in the middle lobe would have higher incidence to be invasive to the upper or lower lobes, so it would be important to explore the whole thoracic cavity before the lobectomy. The uniportal VATS middle lobectomy through 5th intercostal space was a standard procedure. The dissection of the middle lobe pulmonary vein usually came as the first structure, while the identification and dissection of the vein remained challenging using endoscopic staplers. Because the stapler had a restricted curve to pass through both the incision and the middle pulmonary vein, while the ligation of the vein might be an alternative during the middle lobe lobectomy. The surgery went on sequentially with the dissection of middle lobe bronchus and the artery.
The specimen was taken out in the specimen bag (Ethicon Endo-Surgery Inc, Cincinnati, OH, USA). In the cases of large size tumor, Dr. Sihoe from Hong Kong SAR suggested to dissect one rib to facilitate the take-out, which would be an alternative during the uniportal VATS lobectomy. A 28-Fr chest tube was inserted at the end of the operation, and the chest tube would be removed in the cases there was no air leakage and the volume of drainage was less than 200 mL per day 24 hours post-operatively.
Conversions
In multiportal VATS, the conversion to thoracotomy was not considered as the failure of the procedure. Meanwhile, the uniportal VATS required learning curve to reach a stable plateau of performance. Therefore, the application of additional port or even thoracotomy would be helpful when the operation ran into difficulty. The severe thoracic adhesion, major bleeding or lymph node invasion could be the main reasons to do the conversion.
Learning curve
Every surgical procedure required certain case volumes to reach the plateau of performance. At this point, the uniportal VATS lobectomy was not an exceptional. As most surgeons turned to uniportal VATS could have some experience on minimally invasive surgery, the difficulty relied mostly on how to pass the staplers through the inter-space among the mediastinal vessels. Sometimes the lobe should be contracted towards different directions to match the endo-cutter, and the assistant surgeon would therefor play an important role throughout the surgery. Since the surgeon and the assistant stood at the same side during the operation, with the better training opportunities, the learning curve for this demanding procedure might be shortened in spite of the difficulties mentioned above.
Future prospective
Uniportal VATS, is not the happy ending in thoracic surgery. Beside its rapid progression, there remained a lot of questions to answer. Its uncovered benefits and drawbacks over traditional VATS, its possible improvements, and less invasive peri-operative managements could be the future topics. A comparison between uniportal versus multiportal VATS using high-level methodology is therefore required. With the development of surgical minds and instruments, uniportal VATS would have done more to the patients.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The study was approved by the Ethics Committee of Zhongshan Hospital, Fudan University. Written informed consent was obtained from the patient. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
References
- Rocco G, Martin-Ucar A, Passera E. Uniportal VATS wedge pulmonary resections. Ann Thorac Surg 2004;77:726-8. [PubMed]
- Gonzalez-Rivas D, Paradela M, Fernandez R, et al. Uniportal video-assisted thoracoscopic lobectomy: two years of experience. Ann Thorac Surg 2013;95:426-32. [PubMed]
- Gonzalez D, de la Torre M, Paradela M, et al. Video-assisted thoracic surgery lobectomy: 3-year initial experience with 200 cases. Eur J Cardiothorac Surg 2011;40:e21-8. [PubMed]
- Gonzalez-Rivas D, Fernandez R, Fieira E, et al. Uniportal video-assisted thoracoscopic bronchial sleeve lobectomy: first report. J Thorac Cardiovasc Surg 2013;145:1676-7. [PubMed]
- Sihoe AD. The evolution of minimally invasive thoracic surgery: implications for the practice of uniportal thoracoscopic surgery. J Thorac Dis 2014;6:S604-17. [PubMed]
- Wang BY, Liu CY, Hsu PK, et al. Single-incision versus multiple-incision thoracoscopic lobectomy and segmentectomy: a propensity-matched analysis. Ann Surg 2015;261:793-9. [PubMed]
- Anile M, Diso D, Mantovani S, et al. Uniportal video assisted thoracoscopic lobectomy: going directly from open surgery to a single port approach. J Thorac Dis 2014;6:S641-3. [PubMed]
- Shen Y, Liu Y, Feng M, et al. Uniportal VATS upper lobectomy with mediastinal lymph node dissection. Asvide 2015;2:051. Available online: http://www.asvide.com/articles/507
- Liu L, Che G, Pu Q, et al. A new concept of endoscopic lung cancer resection: Single-direction thoracoscopic lobectomy. Surg Oncol 2010;19:e71-7. [PubMed]
Cite this article as:Shen Y, Liu Y, Feng M, Wang H, Tan L, Xi Y, Wang Q. Uniportal video-assisted thoracoscopic lobectomy: Zhongshan experience. J Vis Surg 2015;1:5.