Robot-assisted intrathoracic lymph node dissection for esophagectomy
Introduction
Esophageal cancer is a lethiferous malignancy and a major cause of cancer-related deaths globally. It ranks the seventh in terms of incidence (572,000 new cases) and sixth in mortality (509,000 deaths) in 2018 world-widely (1). The 5-year overall survival rate is approximately 50% in some Japanese series (2) and about 25% in some western countries (3). Despite the advance of radiation and chemotherapy, surgery remains the main treatment of esophageal cancer. The most two important factors affecting the prognosis of esophageal cancer are depth of carcinoma invasion and lymph node metastasis. Lymph node dissection is an essential part of radical surgery as esophageal cancer correlate with a high rate of nodal and distant metastasis. With the development of high-definition surgical imaging systems and surgical instruments, minimally invasive esophagectomy (MIE) has gained much attention in the past two decades.
Since the introduction of robotic system in esophageal surgery in 2000, the number of robotic esophagectomies has been gradually increasing around the world. Studies comparing MIE and open surgery showed MIE patients had more lymph nodes retrieved and shorter hospital stays. But the exact impact and result of robotic system in the lymph node dissection for esophagectomy is still unclear. The aim of this review is to discuss issues with the intrathoracic lymph node dissection and the role of robotic system in the intrathoracic lymph node dissection for esophagectomy.
Thoracic lymph node metastasis pattern
The esophagus can be anatomically divided into three parts, which locate in three compartments of the body. The lymphatic drainage system of the esophagus is very complex and widely distributed in the neck, thorax and upper abdominal region. The upper third of the esophagus drains into the deep cervical lymph nodes, the middle into the superior and posterior mediastinal lymph nodes, and the lower esophagus into the gastric and celiac lymph nodes. The lymphatic drainages are all connected by transverse transmural lymphatic vessels and longitudinal lymphatic vessels in the submucosa and lamina propria. So the unique pattern of the lymph node metastasis can happen in any lymph node from the neck to the abdomen (4). Studies show that lymph node metastasis is frequently seen in the lower neck, upper mediastinum, and perigastric area, even for early-stage thoracic esophageal cancer (5,6). The lymph node metastasis rate varies mainly depending on the location, size, and depth of invasion of the primary tumor. Lymph node metastasis is an independent prognostic factor for esophageal cancer, especially the number or ratio of involved nodes (7-9).
Since the 19th century, the importance of the clearance of the regional lymph nodes in the treatment of the esophageal cancer has been gradually realized by accumulation of practical experiences and knowledge. In the 1960s, Logan (10) reported the role of the mediastinal node dissection in esophagectomy. Later in the 1970s, Sannohe et al. (11) first conducted the lymph node dissection of 36 patients with the thoracic esophageal cancer in bilateral supraclavicular, right intrathoracic and abdominal regions.
Minimally invasive mediastinal lymph node dissection
According to the AJCC system, the mediastinal lymph nodes include the upper right and left paratracheal lymph nodes, upper thoracic paraesophageal lymph nodes, right and left lower paratracheal lymph nodes, subcarinal lymph nodes, middle and lower thoracic paraesophageal lymph nodes, right and left lower pulmonary ligament lymph nodes and paradiaphragmatic lymph nodes.
The selection of the surgical approach largely impacts the number and extent of lymph nodes dissected in radical esophagectomy. Using traditional surgical approach with a left posterolateral thoracic incision, it is difficult to dissect the left and right recurrent laryngeal nerve (RLN) nodes because of the obstacles presented by the aortic arch, left common carotid artery and subclavian artery. While approaches through a right thoracic incision such as Ivor Lewis and McKeown procedures can help overcome this problem. Therefore, these two procedures have gradually become the preferred approaches for thoracic esophageal cancer (12-15).
Due to the high complication rate of conventional esophageal cancer surgery, multiple minimally invasive approaches have been explored to reduce the surgical morbidity and mortality. Several studies showed minimally invasive esophageal surgery presents decreased rates of pneumonia, shorter length of stay, less pain while achieving an appropriate resection, lymph node dissection and similar short-term survival compared to open esophagectomy (16-18). However, MIE has several intrinsic limitations, such as 2-dimensional view, reduced eye-hand coordination and decreased degrees of freedom of movement, which impede the mediastinal dissection and anastomosis during thoracoscopic esophagectomy. Robotic systems can perfectly overcome these disadvantages of standard minimally invasive surgery. The first case of robot-assisted esophagectomy for esophageal carcinoma was reported in 2003 by Dr. Horgan (19). In 2010, Dr. Kim reported 21 cases of RAMIE to verify the feasibility and safety of the McKeown approach (20). The high-definition monitor and three-dimensional vision of the robotic system provide extreme detail and clarity. Moreover, the seven degrees of freedom from the articulating wrists largely facilitate circumferential dissection of the esophagus and surrounding structure. Furthermore, the robotic instruments are 7.5 cm longer than standard laparoscopic instruments, which make it possible to operate in places where most laparoscopic instruments and visualization are at their limits.
Various studies have shown the superiority of robot-assisted lymph node dissection in esophagectomy compared with thoracoscopic esophagectomy. In 2012, Suda et al. showed that robot assistance significantly reduced the incidence of vocal cord palsy and hoarseness (21). In 2016, Park et al. compared the short-term outcomes between RAILE and TAILE and found that the robotic system enabled a more radical lymphadenectomy, especially in the upper mediastinum (22). In 2017, a comparative study from the University of Pittsburgh with their early RAILE experience suggested increased number of LN harvested with RAILE compared with TAILE.
Other studies showed similar results of RAMIE and TAMIE. In 2012, Weksler reported no significant differences in number of resected lymph nodes between the two surgical approaches (23). In 2018, He et al. reported comparable results between RAMIE and TAMIE in the number of total dissected lymph nodes as well as the incidence of RLN injury (24).
We retrospectively analyzed data of 184 patients from our hospital, 76 in the RAILE group and 108 in the TAILE group, who underwent minimally invasive Ivor-Lewis esophagectomy between December 2014 and June 2018. And preliminary results showed no significant difference in blood loss, rates of overall complications, number of total dissected lymph nodes and detailed categories of lymph nodes.
RLN lymph node dissection
Among all the mediastinal lymph nodes, the lymph nodes around RLN, which are located at the junction of the neck and chest, are important for thoracic esophageal cancer (25,26). Numerous studies have reported the high risk of metastasis to the lymph nodes near both sides of RLN. Ye et al. reported the rate of LN metastasis near the bilateral RLN was 34.2%, in which 15.8% involving the left LNs and 20.8% involving the right LNs (27). Kato et al. (28) found the right RLN lymph nodes were the most frequent site of lymph node metastasis. Fujita et al. (29) reported left RLN lymph nodes being the most frequent lymph node recurrence after operation. Therefore, it is necessary to perform a radical lymph node dissection on both RLN during thoracic surgery to achieve accurate pathological staging and complete tumor eradication. The RLN lymph node acts as a strong indicator of cervical lymph node metastasis and an important factor regarding the postoperative survival rate of patients with esophageal cancer (27,30).
Injuries to the RLNs are frequently seen and often result in recurrent laryngeal nerve palsy (RLNP). Careful exposure and avoidance of thermal injury, stretching and compression of the RLN can help prevent RLNP. It is suggested to start the dissection begin from where the right RLN branches off from the vagus nerve and the left recurrent nerve curves around the aortic arch.
The robotic system provided great accessibility for the subtle manipulations, especially while dissecting lymph nodes around the RLNs. In 2012, a randomized controlled trial showed the rate of RLN injury was significantly lower in the MIE group (31). In 2018, Chao et al. showed that robotic esophagectomy resulted in a higher lymph node LN yield along the left RLN with similar results regarding mean number of dissected nodes and rates of RLNP (32). Kim et al. reported that robot-assisted skeletonization of the RLNs yields more lymph nodes, but also leads to more incidence of RLNP (33). In general, robot-assisted thoracoscopic lymphadenectomy along bilateral RLNs was technically feasible and safe. Table 1 shows the summary of the studies quoted in this review.
Table 1
| Author | No. of cases | Operative time (min) | Blood loss (mL) | Hospital stay (days) | No. of dissected lymph nodes | Complications (%) | OCEBM level of evidence | Grade of recommendation | ||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Total | Thoracic phase | Total | Mediastinal | Vocal cord palsy | Pulmonary complications | |||||||
| Kim |
21 | 410 | NR | 150 | 21 | 32.7 | 11.6 | 28.6 | 0 | 2b | B | |
| Suda |
16 | 693 | 336 | 144.5 | 22 | 37.5 | 18.5 | 37.5 | 6.3 | 2b | B | |
| Park |
62 | 490 | 185 | 462 | NR | 37.3 | 24.9 | 12.9 | 14.5 | 2b | B | |
| Weksler |
11 | 439 | NR | 200 | 8.7 | 23.0 | NR | 9.1 | 27.3 | 2a | B | |
| He |
27 | 349 | NR | 118 | 13.8 | 20.0 | NR | 14.8 | 18.5 | 2b | B | |
| Chao |
37 | NR | 198 | 115 | 20.6 | 34.4 | 17.6 | 21.6 | 8.1 | 2b | B | |
| Kim |
40 | 429 | NR | 157 | 14 | 42.6 | 25.5 | 20.0 | 12.5 | 2a | B | |
NR, not reported.
Videos of robot-assisted right RLN lymph node dissection (Figure 1) and left RLN lymph node dissection (Figure 2) for esophagectomy are present here. During the right RLN lymph node dissection, the mediastinal pleura were first divided to reveal the trachea and subclavian artery. Then we dissected along the right vagus nerve to find its right RLN branch at the dorsal of subclavian artery and obtain the lymph nodes. When dissecting the left RLN lymph nodes, the trachea was pushed aside by the assistant, and the esophagus was pulled upward to expose the surgical field. Then the left RLN was clearly seen by careful blunt dissection and the lymph nodes were harvested. It is considered that single lumen intubation can facilitate with a good exposure.


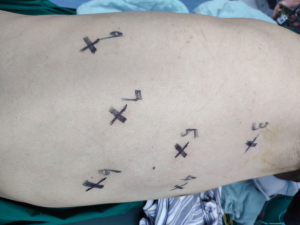
The thoracic ports are shown in Figure 3. The approximate positions are described below. The observation port was placed on the right anterior axillary line at the 5th intercostal space, the #1 robotic arm was placed on the right midaxillary line at the 3th intercostal level, the #3 robotic arm was placed on the right posterior axillary line at 9th intercostal space, the #2 robotic arm was placed between #1 and #3 robotic arm at 7th intercostal space, and the manual operative ports were placed at the 4th and 6th intercostal space.
Lymphadenectomy-related complications
Mediastinal lymphadenectomy of esophageal cancer may lead to intensive trauma because of extensive surgical dissection. Some of the postoperative complications are associated with lymphadenectomy in esophagectomy (36). Meticulous dissection is required to avoid injury to the important organs such as the aorta, pulmonary vessels, trachea, RLN, and thoracic duct.
Damage to the membranous trachea or the main bronchus may occur when dissecting the paratracheal and subcarinal lymph nodes. Energy devices such as electric cautery or harmonic scalpel should be carefully used to avoid thermal damage to the tracheal membrane. It is better to employ the energy devices with intermittent cooling to avoid overheating.
Pulmonary complication such as pneumothorax, pneumonia and atelectasis, is a leading cause of mortality after esophagectomy. Overstretching or compressing of the lung parenchyma may lead to pulmonary injuries such as congestion or rupture of the lung. When dissecting the subcarinal lymph nodes, careful management of the bronchial arteries and the pulmonary branches of the vagus nerves may help prevent some complications associated with pulmonary injury. Postoperative management such as transfusion volume and use of antibiotics is also crucial in the development of pulmonary complications.
Chylothorax is another potentially lethal complication which might be caused by extensive lymphadenectomy (37,38). Injuries to large lymphatic tributaries or the thoracic duct may cause refractory chylothorax. Some researchers claim it is better to dissect and expose the thoracic duct clearly during mediastinal lymphadenectomy. Thoracic duct ligation near the hiatus should be performed if injury is suspected.
The initial intent of MIE is to reduce the high incidence of complications. Review of the literature shows a substantial decrease in postoperative complications with comparable oncologic results (39,40). In 2016, a meta-analysis of 1,549 cases by Guo et al. found that MIE led to fewer postoperative complications and a similar survival rate when compared to open surgery (41). Biere et al. showed MIE resulted in a lower incidence of in-hospital pulmonary infections, a shorter hospital stay and better short-term quality of life than open esophagectomy (31).
Conclusions
Intrathoracic lymph node dissection is crucial in radical treatment of esophageal cancer. The application of robotic technology in intrathoracic lymph node dissection for esophagectomy has proven to be at least comparable and to some extent, superior to open or video assisted thoracoscopic techniques. By virtue of the 3D camera, articulating wrists and improved dexterity of the robotic system, surgeons are capable of performing delicate esophagectomy and lymph node dissection, especially around the RLNs. It is reported that robotic surgery can achieve more satisfactory outcomes of local lymph node dissection in the superior mediastinum with less perioperative complications. However, definitive evidence supporting the superiority of robotic esophagectomy regarding morbidity and mortality is still lacking. Moreover, the current results may be influenced by the choice of surgical techniques and the learning curve of surgeons. The high cost of robot surgery may also hinder its popularity. More studies with larger cohorts and higher levels of evidence are needed to assess the long term results of robot-assisted esophagectomy in the future. Overall, the application of robotic system in intrathoracic lymph node dissection of esophagectomy is reliable and satisfactory. With the advance of surgical instruments and the development of training programs, patients will benefit more from robot-assisted esophagectomy.
Acknowledgments
Funding: This study was supported by the grant from Shanghai Municipal Education Commission-Gaofeng Clinical Medicine Grant Support (20172005), Shanghai Municipal Commission of Health and Family Planning Outstanding Academic Leaders Training Program (2017BR055) and Intuitive Surgical Clinical Research Grant.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editor (Abbas E. Abbas) for the series “Robotic Surgery for Esophageal Cancer” published in Journal of Visualized Surgery. The article has undergone external peer review.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jovs.2019.05.06). The series “Robotic Surgery for Esophageal Cancer” was commissioned by the editorial office without any funding or sponsorship. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Bray F, Ferlay J, Soerjomataram I, et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 2018;68:394-424. [Crossref] [PubMed]
- Nakagawa S, Kanda T, Kosugi SI, et al. Recurrence pattern of squamous cell carcinoma of the thoracic esophagus after extended radical esophagectomy with three-field lymphadenectomy. J Am Coll Surg 2004;198:205-11. [Crossref] [PubMed]
- Daly JM, Fry WA, Little AG, et al. Esophageal cancer: results of an American College of Surgeons patient care evaluation study11No competing interests declared. J Am Coll Surg 2000;190:562-72. [Crossref] [PubMed]
- Fujita H, Kakegawa T, Yamana H, et al. Lymph node metastasis and recurrence in patients with a carcinoma of the thoracic esophagus who underwent three-field dissection. World J Surg 1994;18:266-72. [Crossref] [PubMed]
- Akutsu Y, Uesato M, Shuto K, et al. The overall prevalence of metastasis in T1 esophageal squamous cell carcinoma: a retrospective analysis of 295 patients. Ann Surg 2013;257:1032-8. [Crossref] [PubMed]
- Hölscher AH, Bollschweiler E, Schroder W, et al. Prognostic impact of upper, middle, and lower third mucosal or submucosal infiltration in early esophageal cancer. Ann Surg 2011;254:802-7; discussion 807-8. [Crossref] [PubMed]
- Sugawara K, Yamashita H, Uemura Y, et al. Numeric pathologic lymph node classification shows prognostic superiority to topographic pN classification in esophageal squamous cell carcinoma. Surgery. 2017;162:846-56. [Crossref] [PubMed]
- Zhang H, Liang H, Gao Y, et al. Metastatic lymph node ratio demonstrates better prognostic stratification than pN staging in patients with esophageal squamous cell carcinoma after esophagectomy. Sci Rep 2016;6:38804. [Crossref] [PubMed]
- Shao Y, Geng Y, Gu W, et al. Assessment of lymph node ratio to replace the pN categories system of classification of the TNM system in esophageal squamous cell carcinoma. J Thorac Oncol 2016;11:1774-84. [Crossref] [PubMed]
- Logan A. The surgical treatment of carcinoma of the esophagus and cardia. J Thorac Cardiovasc Surg 1963;46:150-61. [PubMed]
- Sannohe Y, Hiratsuka R, Doki K. Lymph node metastases in cancer of the thoracic esophagus. Am J Surg 1981;141:216-8. [Crossref] [PubMed]
- Wang ZQ, Deng HY, Hu Y, et al. Prognostic value of right upper mediastinal lymphadenectomy in Sweet procedure for esophageal cancer. J Thorac Dis 2016;8:3625-32. [Crossref] [PubMed]
- Li B, Xiang J, Zhang Y, et al. Comparison of Ivor-Lewis vs Sweet esophagectomy for esophageal squamous cell carcinoma: a randomized clinical trial. JAMA Surg 2015;150:292-8. [Crossref] [PubMed]
- Duan X, Shang X, Tang P, et al. Lymph node dissection for Siewert II esophagogastric junction adenocarcinoma: a retrospective study of 136 cases. ANZ J Surg 2018;88:E264-E267. [Crossref] [PubMed]
- Li B, Hu H, Zhang Y, et al. Extended right thoracic approach compared with limited left thoracic approach for patients with middle and lower esophageal squamous cell carcinoma: Three-year survival of a prospective, randomized, open-label trial. Ann Surg 2018;267:826-32. [Crossref] [PubMed]
- Lv L, Hu W, Ren Y, et al. Minimally invasive esophagectomy versus open esophagectomy for esophageal cancer: a meta-analysis. Onco Targets Ther 2016;9:6751-62. [Crossref] [PubMed]
- Kauppila JH, Helminen O, Kytö V, et al. Short-term outcomes following minimally invasive and open esophagectomy: A Population-Based Study from Finland and Sweden. Ann Surg Oncol 2018;25:326-32. [Crossref] [PubMed]
- Luketich JD, Pennathur A, Awais O, et al. Outcomes after minimally invasive esophagectomy: review of over 1000 patients. Ann Surg 2012;256:95-103. [Crossref] [PubMed]
- Horgan S, Berger RA, Elli EF, et al. Robotic-assisted minimally invasive transhiatal esophagectomy. Am Surg 2003;69:624-6. [PubMed]
- Kim DJ, Hyung WJ, Lee CY, et al. Thoracoscopic esophagectomy for esophageal cancer: feasibility and safety of robotic assistance in the prone position. J Thorac Cardiovasc Surg 2010;139:53-59.e1. [Crossref] [PubMed]
- Suda K, Ishida Y, Kawamura Y, et al. Robot-assisted thoracoscopic lymphadenectomy along the left recurrent laryngeal nerve for esophageal squamous cell carcinoma in the prone position: Technical report and short-term outcomes. World J Surg 2012;36:1608-16. [Crossref] [PubMed]
- Park S, Hwang Y, Lee HJ, et al. Comparison of robot-assisted esophagectomy and thoracoscopic esophagectomy in esophageal squamous cell carcinoma. J Thorac Dis 2016;8:2853-61. [Crossref] [PubMed]
- Weksler B, Sharma P, Moudgill N, et al. Robot-assisted minimally invasive esophagectomy is equivalent to thoracoscopic minimally invasive esophagectomy. Dis Esophagus 2012;25:403-9. [Crossref] [PubMed]
- He H, Wu Q, Wang Z, et al. Short-term outcomes of robot-assisted minimally invasive esophagectomy for esophageal cancer: a propensity score matched analysis. J Cardiothorac Surg 2018;13:52. [Crossref] [PubMed]
- Wang F, Zheng Y, Wang Z, et al. Nodal skip metastasis in esophageal squamous cell carcinoma patients undergoing three-field lymphadenectomy. Ann Thorac Surg 2017;104:1187-93. [Crossref] [PubMed]
- Liu J, Liu Q, Wang Y, et al. Nodal skip metastasis is associated with a relatively poor prognosis in thoracic esophageal squamous cell carcinoma. Eur J Surg Oncol 2016;42:1202-5. [Crossref] [PubMed]
- Ye K, Xu JH, Sun YF, et al. Characteristics and clinical significance of lymph node metastases near the recurrent laryngeal nerve from thoracic esophageal carcinoma. Genet Mol Res 2014;13:6411-9. [Crossref] [PubMed]
- Kato H, Tachimori Y, Mizobuchi S, et al. Cervical, mediastinal, and abdominal lymph node dissection (threefield dissection) for superficial carcinoma of the thoracic esophagus. Cancer 1993;72:2879-82. [Crossref] [PubMed]
- Fujita H, Kakegawa T, Yamana H, et al. Lymph node metastasis and recurrence in patients with a carcinoma of the thoracic esophagus who underwent three-field dissection. World J Surg 1994;18:266-72. [Crossref] [PubMed]
- Hou X, Wei JC, Fu JH, et al. Proposed modification of the seventh American Joint Committee on Cancer Staging System for esophageal squamous cell carcinoma in Chinese patients. Ann Surg Oncol 2014;21:337-42. [Crossref] [PubMed]
- Biere SS, van Berge Henegouwen MI, Maas KW, et al. Minimally invasive versus open oesophagectomy for patients with oesophageal cancer: a multicentre, open-label, randomised controlled trial. Lancet 2012;379:1887-92. [Crossref] [PubMed]
- Chao YK, Hsieh MJ, Liu YH, et al. Lymph node evaluation in robot-assisted versus video-assisted thoracoscopic esophagectomy for esophageal squamous cell carcinoma: A propensity-matched analysis. World J Surg 2018;42:590-8. [Crossref] [PubMed]
- Kim DJ, Park SY, Lee S, et al. Feasibility of a robot-assisted thoracoscopic lymphadenectomy along the recurrent laryngeal nerves in radical esophagectomy for esophageal squamous carcinoma. Surg Endosc 2014;28:1866-73. [Crossref] [PubMed]
- Gan Q, Han D, Li H. Robot-assisted Ivor-Lewis esophagectomy dissection of lymph nodes along right recurrent laryngeal nerve. Asvide 2019;6:185. Available online: http://www.asvide.com/article/view/32482
- Gan Q, Han D, Li H. Robot-assisted Ivor-Lewis esophagectomy dissection of lymph nodes along left recurrent laryngeal nerve. Asvide 2019;6:186. Available online: http://www.asvide.com/article/view/32483
- Sharma S. Management of complications of radical esophagectomy. Indian J Surg Oncol 2013;4:105-11. [Crossref] [PubMed]
- Brinkmann S, Schroeder W, Junggeburth K, et al. Incidence and management of chylothorax after Ivor Lewis esophagectomy for cancer of the esophagus. J Thorac Cardiovasc Surg 2016;151:1398-404. [Crossref] [PubMed]
- Shah RD, Luketich JD, Schuchert MJ, et al. Postesophagectomy chylothorax: incidence, risk factors, and outcomes. Ann Thorac Surg 2012;93:897-903; discussion 903-4. [Crossref] [PubMed]
- Verhage RJ, Hazebroek EJ, Boone J, et al. Minimally invasive surgery compared to open procedures in esophagectomy for cancer: a systematic review of the literature. Minerva Chir 2009;64:135-46. [PubMed]
- Nafteux P, Moons J, Coosemans W, et al. Minimally invasive oesophagectomy: a valuable alternative to open oesophagectomy for the treatment of early oesophageal and gastro-oesophageal junction carcinoma. Eur J Cardiothorac Surg 2011;40:1455-63; discussion 1463-4. [PubMed]
- Guo W, Ma X, Yang S, et al. Combined thoracoscopic-laparoscopic esophagectomy versus open esophagectomy: a meta-analysis of outcomes. Surg Endosc 2016;30:3873-81. [Crossref] [PubMed]
Cite this article as: Gan Q, Han D, Li H. Robot-assisted intrathoracic lymph node dissection for esophagectomy. J Vis Surg 2019;5:59.