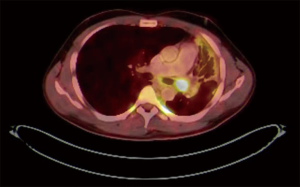
Robotic resection of inflammatory tumour
Introduction
Inflammatory diseases are prevalent in Asian Subcontinent, particularly in South East Asia. They cause severe inflammatory responses and dense adhesionsin the chest. This is one of the reasons why video assisted and robotic thoracic surgery took time to gain a foothold in countries like India, Pakistan, Nepal and Bangladesh. It is very difficult to promote VATS/Robotic surgery as It is technically very challenging to enter a densely adherent chest.
We present our experience with starting and setting up a minimally invasive robotic thoracic surgery program in India in the background of endemic tuberculosis and inflammatory diseases.
Case presentation
A 26-year-old patient presented to us from Bangladesh with a history of recurrent chest infections. He was treated with repeated courses of antibiotics. Chest X-ray showed collapse and consolidation of left upper lobe with progressive collapse of lower lobe. He was also started on an empirical course of Anti tuberculosis therapy. This is unfortunately a common practise in South East Asia tuberculosis is endemic. Since he was showing no improvement, he as referred to us for a tertiary opinion.
PET CT scan showed the presence of an endobronchial tumour in the left main bronchus (Figure 1). There was some aeration of left lower lobe with a collapse consolidated upper lobe. Endobronchial Biopsy was haemorrhagic. Histopathology suggested the presence of chronic inflammatory cells with no evidence of malignancy. Acid fast bacilli were negative on microscopy and culture. A preliminary diagnosis of endobronchial inflammatory tumour was made and he was scheduled for Robotic resection of Lung.
Intraoperative strategy
A preoperative rigid bronchoscopy was performed. It was mandatory for us to try and avoid a pneumonectomy as this was only an inflammatory process with no evidence of malignancy. The growth seemed to arise from the left upper lobe and encroach onto the left main bronchus. It seemed that the lower lobe bronchus was blocked due to prolapsing tumour rather than infiltration.
We used a Da Vince Si Robotic platform to perform the surgery. The ports are placed in a linear fashion along the 6th Intercostal space with a distance of 9 cm between the ports. With the newer Xi system, you could reduce the space between the ports. A additional port was paced in the 10th intercostal space for assistance and to deliver the stapler. With SI system, you do not have the ability to perform Robotic stapling. With Xi system, this is an added benefit, hence you may not need an assistant port.
The surgery was started with VATS to enable us to do some dissection of adhesions and create the space to dock the robot.
Once the robot is docked after the three ports are created, we dissected the adhesions under vision (Figure 2). This prevents bleeding. The pulmonary vein to upper love was dissected and stapled using a standard white stapler. The arterial branches to upper lobe were identified, dissected and stapled. The bronchus to upper lobe was isolated. A bronchotomy was made in the bronchus using a robotic scissor. The tumour was delivered out from the bronchotomy. An intraoperative bronchoscopy was performed to ensure complete removal of all tumour from lower lobe. Complete Endobronchial suctioning and toil was performed. Since we were dealing with an inflammatory tumour, we did not need to send the margins for frozen section. The upper lobe was resected and delivered out in a bag. The Margins of the upper lobe bronchus was sutured with 3-0 PDS suture. Use of robotics platform makes the suturing very easy and intuitive. Suturing by VATS is technically more challenging as we are dealing with a mirror image. Intraoperative lung expansion and under water test was performed to ensure no air leak. A single drain was placed and connected to a suction bottle at –2 Kpas. An extrapleural catheter was sited for pain control.

Postoperative recovery
The drain was removed on day 2 post op. Aggressive chest physiotherapy and Yoga therapy was initiated. Chest X-ray confirmed good lung expansion. The patient was discharged on 3rd postoperative day.
Follow up
This patient was followed up for 2 years now and has confirmed good lung expansion. Clinically he is doing well with no symptoms. He is not short of breath and has no recurrence of chest infection. A follow up bronchoscopy was not required as the patient was clinically well.
Discussion
Robotics thoracic surgery in inflammatory diseases (2) offered us the following benefits:
- High definition optics and 3D visualisation of intrathoracic anatomy and structures;
- 360-degree movement and 7 degree of freedom for Endowrist;
- Ability to dissect adhesions under vision thereby reducing the blood loss;
- Ability to dissect carefully under direct vision around major vascular structures;
- Ability to do a bronchotomy and deliver the tumour out so that the lower lobe +/– upper lobe could be spared;
- The ability to suture the bronchus intuitively or perform a sleeve anastomosis.
The other benefits were similar to VATS and included the following:
- Smaller incisions;
- No muscle cutting;
- No spreading of ribs;
- Less inflammatory response (3);
- Less immunological response (3);
- Shorter hospital-stay (4,5);
- Quicker return to work (3-5);
- Less damage to the chest wall muscles thereby better post operative respiratory reserve and function leading to less atelectasis and chest infection (4-6);
- Less pain hence better compliance with post operative chest physiotherapy (6);
- Earlier mobilisation hence less psychological effects;
- Better cosmetic results (4).
Conclusions
We conclude that using robotics in challenging inflammatory diseases is technically possible. The ease of suturing on the robotic platform makes sleeve resection technically possible by minimally invasive surgery. We can achieve good clinical outcomes and early discharge from hospital.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the editorial office, Journal of Visualized Surgery for the series “Asia Thoracoscopic Surgery Education Program (ATEP) Special Issue on Inflammatory Thoracic Diseases”. The article has undergone external peer review.
Conflicts of Interest: Both authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jovs.2019.02.05). The series “Asia Thoracoscopic Surgery Education Program (ATEP) Special Issue on Inflammatory Thoracic Diseases” was commissioned by the editorial office without any funding or sponsorship. KA served as the unpaid Guest Editor of the series. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in studies involving human participants were in accordance with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Khan AZ, Ali K. Robotic sleeve lobectomy for inflammatory tumour of left lung. Asvide 2019;6:090. Available online: http://www.asvide.com/article/view/30914
- Sihoe AD, Shiraishi Y, Yew WW. The current role of thoracic surgery in tuberculosis management. Respirology 2009;14:954-68. [Crossref] [PubMed]
- Yim AP, Izzat MB, Lee TW. Thoracoscopic surgery for pulmonary tuberculosis. World J Surg 1999;23:1114-7. [Crossref] [PubMed]
- Yim AP. The role of video-assisted thoracoscopic surgery in the management of pulmonary tuberculosis. Chest 1996;110:829-32. [Crossref] [PubMed]
- Kandwal P, Garg B, Upendra B, et al. Outcome of minimally invasive surgery in the management of tuberculous spondylitis. Indian J Orthop 2012;46:159-64. [Crossref] [PubMed]
- Yablonskii P, Kudriashov G, Vasilev I, et al. Robot-assisted surgery in complex treatment of the pulmonary tuberculosis. J Vis Surg 2017;3:18. [Crossref] [PubMed]
Cite this article as: Khan AZ, Ali K. Robotic resection of inflammatory tumour. J Vis Surg 2019;5:34.