
Port-access thoracoscopic anatomical left S3 segmentectomy
Introduction
The indications for video-assisted thoracic surgery (VATS) segmentectomy are growing with the significant advancements in surgical techniques. However, this procedure seems to be limited for anatomically simple and easy procedures such as left upper division, lingular (S4+5) and S6 segmentectomies. Intersegmental dissection in such segmentectomies is not procedurally difficult, because the dissection can simply be performed by using stapling devices along the single intersegmental plane.
We present the surgical procedure for VATS anatomical left S3 segmentectomy according to the simulation of surgical margin and bronchovascular branching using three-dimensional (3D) computed tomography (CT) reconstruction.
Procedure
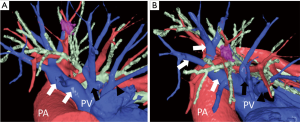
Resection of left S3 was planned as the nodule was located between the subsegmental bronchi. The bronchovascular branching pattern was identified under precise assessment of 1-mm sliced axial images and 3D reconstruction of multidetector CT data (Figure 1). Standard anesthesia for thoracic surgery was performed with a double lumen endotracheal tube and general anesthesia. The patient was placed in a lateral position with the left upper extremity fixed onto the hand shelf. The surgeon stood in an anterior position to the patient.
Two flexible 5-mm ports and one 20-mm soft silicone port were inserted, and a 30° 10-mm rigid scope was used. We first incised the lung parenchyma along the V1+2 that runs between S1+2 and S3, then the V3b that runs between S3 and S4. The hilum of S3 was exposed and we isolated and divided the vein V3c that runs into the affected segment. In this patient, as the first branch of left pulmonary artery was composed of anterior artery (A3) and lingular artery (A4+5) the A3 was isolated from the A4+5 branch and ligation and division were done. The anterior segmental bronchus (B3) was looped using a monofilament polypropylene thread. A slip knot was made using the thread outside her thorax, and bilateral pure oxygen lung ventilation was performed. During the lung ventilation, the end of the thread was pulled, and the knots slipped to reach the bronchus without a knot pusher so as to trap the segmental air of the S3. The unilateral ventilation was resumed and the B3 was divided using a stapler, then dissection of hilar parenchyma was done dividing venous branches running into the segments. During this procedure, the inflation-deflation lines between the segments gradually become apparent. We further incised the lung parenchyma along the inflation-deflation line and finally the peripheral lung was divided using staplers. Fibrin glue was sprayed at the remnant cut surface (Figure 2) (1). The operative time was 152 min. The estimated blood loss was 4 mL. Air leakage was not observed, and the chest tube was removed at the first postoperative day. The final diagnosis was a lepidic adenocarcinoma. She lives well without recurrence 42 months after the left lung operation.

Comments
We previously reported the thoracoscopic anatomical segmentectomy under the use of 3D reconstruction of multidetector row CT of the affected segments and so far, performed 335 procedures including 10 right and 7 left S3 segmentectomies. To perform the anatomical segmentectomy procedure, precise understanding of hilar bronchovascular anatomy is important under the use of multidetector CT data (2,3). As for the left S3 segmentectomy, we first catch the anatomy of V3 as the branches usually run between left upper division and lingular segment, then put weight on the running of V1+2 that runs between apical posterior segment (S1+2) and S3 under precise assessment of 1-mm sliced axial images as well as the 3D reconstruction of multidetector CT data. Anterior artery (A3) and bronchus (B3) are usually identifiable between these two veins. Thus, during the S3 segmentectomy, we first identify these veins at the hilum and dissect the lung parenchyma towards peripheral using energy sealing devices such as ultrasonically activated device or along the intersegmental veins and isolate A3 and B3.
It is beneficial to maintain the affected segment inflated for the resection of segment with multiple dissection surfaces. The merit of creating an inflation-deflation line is that the demarcation line does not disappear once it becomes visible. The jet ventilation method is developed for this purpose in thoracoscopic surgery or small thoracotomy (4). However, this method needs an extra equipment and maneuver of a bronchoscope. We developed the slip-knot method that enabled the creation of an inflation-deflation line even in anatomical subsegmental resection of which the bronchial diameter is small (5,6). Although some other methods of visualizing the intersegmental plane (i.e., injection of dye into the target segmental bronchus using a needle or infrared visualization with intravenous injection of indocyanine green) have been reported, some processes may need special equipment or bronchoscopy skill of the anesthetist.
In conclusion, anatomical segmentectomy can be performed under precise recognition of intersegmental veins and creation of inflation-deflation line as intersegmental borders.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editor (Alessandro Brunelli) for the series “Uncommon Segmentectomies” published in Journal of Visualized Surgery. The article has undergone external peer review.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jovs.2018.06.12). The series “Uncommon Segmentectomies” was commissioned by the editorial office without any funding or sponsorship. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Oizumi H, Kato H, Suzuki J, et al. Surgical procedure of thoracoscopic left S3 segmentectomy. Asvide 2018;5:604. Available online: http://www.asvide.com/article/view/25743
- Oizumi H, Kanauchi N, Kato H, et al. Total thoracoscopic pulmonary segmentectomy. Eur J Cardiothorac Surg 2009;36:374-7; discussion 377. [Crossref] [PubMed]
- Oizumi H, Kanauchi N, Kato H, et al. Anatomic thoracoscopic pulmonary segmentectomy under 3-dimensional multidetector computed tomography simulation: a report of 52 consecutive cases. J Thorac Cardiovasc Surg 2011;141:678-82. [Crossref] [PubMed]
- Okada M, Mimura T, Ikegaki J, et al. A novel video-assisted anatomic segmentectomy technique: selective segmental inflation via bronchofiberoptic jet followed by cautery cutting. J Thorac Cardiovasc Surg 2007;133:753-8. [Crossref] [PubMed]
- Oizumi H, Kato H, Endoh M, et al. Slip knot bronchial ligation method for thoracoscopic lung segmentectomy. Ann Thorac Surg 2014;97:1456-8. [Crossref] [PubMed]
- Endoh M, Oizumi H, Kato H, et al. How to demarcate intersegmental plane with resected-segments inflation method using the slip knot technique in thoracoscopic anatomic segmentectomy. J Vis Surg 2017;3:100. [Crossref] [PubMed]
Cite this article as: Oizumi H, Kato H, Suzuki J, Hamada A, Nakahashi K, Sadahiro M. Port-access thoracoscopic anatomical left S3 segmentectomy. J Vis Surg 2018;4:139.


