Thymic minimally invasive surgery: state of the art across the world: Central-South America
Introduction
Thymic malignancies are relatively rare, and evidence supporting the management of such tumors is based only in a few retrospective case series. Surgery is the mainstay treatment and for many years it was performed by the means of open surgery (median sternotomy, clam-shell or antero-lateral thoracotomy). With the development of minimally invasive surgery (MIS), thoracic surgeons started gradually to migrate to less invasive approaches as multiportal video-assisted thoracic surgery (VATS), uniportal VATS or robotic surgery.
Many surgeons have been reluctant to incorporate MIS for treating thymic tumors because of concerns related to tumor seeding and incomplete resection. Nevertheless, a recent meta-analysis of non-randomized case studies demonstrated no difference between open approaches and MIS with regard to complications, rate of R0 resection and recurrence rate (1). This meta-analysis showed an advantage of the MIS approach in terms of blood loss and length of stay, though (1).
Thymic resection has also been performed in order to treat selected cases of myasthenia gravis. This indication was recently confirmed in a randomized clinical trial comparing extended transsternal thymectomy and standard clinical treatment; better outcomes were observed in 3-year follow-up in the surgical group (2). Similarly, to what happened with thymic malignancies, many surgeons had the perception that MIS for thymectomy in myasthenic patients would result in an incomplete procedure. Again, non-randomized evidence suggests that both approaches have equivalent disease control rates, but MIS could be associated with less complications and shorter length of stay (3,4).
VATS adoption in Central and South America is challenging due to budget constraints in health care but also because of training issues. Both these barriers were raised in an e-mail survey carried out in 2015 by the Brazilian Society of Thoracic Surgery (BSTS) (unpublished data). These two factors were considered by most the 225 respondents (active members of the society) as the main causes to prevent a wider adoption of VATS in Brazil. Nevertheless, the high interest on the technique was also clear in the survey results. Considering the rarity of thymic resections and the paucity of high volume referral centers in the region, expanding the use MIS is a complex enterprise. Throughout this paper I will also include Mexico in the discussion, therefore I will refer to the region as Latin America from now on. The objective of this paper is to present the development and current role of MIS for the treatment of thymic diseases in Latin America.
MIS in Latin America
VATS was implemented in Latin America in the early 1990s. In Brazil, the first case series including 488 cases from four centers was published in 1994, and in that series, 35 patients had mediastinal procedures, mostly pericardial windows (5). In the early 2000s, more detailed case series were published by Brazilian surgeons reporting the use of VATS, one focusing in talc poudrage for pleurodesis (611 cases) and the other one in mediastinal lesions (73 patients) (6,7). In the following years, other surgeons from Brazil (8), but also from Argentina (9) and Cuba (10), reported their growing experience with low-complexity mediastinal VATS procedures. Most of these cases were bronchogenic cysts, schwannomas, and thymic cysts. Also in this period, two groups, one from Brazil (11) and the other from Chile (12) reported their initial experience with thymectomy for myasthenia.
There was a big-time lapse since those first initial experiences until the publication of a large series of anatomic lung resections in Brazil (13). In that paper, the authors reported the outcomes of 649 major lung resections performed by 18 thoracic surgeons from 14 institutions from different parts of the country. All members of the BSTS were invited to contribute with this study. The small number of contributors (BSTS has some 600 members, only 18 sent data), the small number of cases per surgeon and the time lapse in the literature demonstrate that the migration for more complex procedures in Brazil was very slow but is gradually happening. A similar scenario is observed in other Latin American countries. We expect that adoption will be faster now because many training centers and academic hospitals teach VATS in their residency programs.
With regard to robotic surgery, in Latin America the technique is in its very early days. The first procedures were performed around 2010 (14) and until recently there were only two active centers, one in Sao Paulo and one in Bogotá. Nonetheless, there is a growing interest in the technique and large academic centers started their programs and one of them has already published its very initial experience (15).
MIS for thymic procedures in Latin America
The first reports on VATS thymic surgery in Latin America were in the early 2000s and described the outcomes of thymectomy for Myasthenia Gravis. In one study (11), the authors performed bilateral VATS and cervicotomy for extended thymus resection in 21 patients. The complication rate and clinical control in the long-term were good. This approach was more frequently used in the past, it is rarely used nowadays, since it is possible to carry out an extended thymic resection even from a uniportal VATS, thus avoiding multiple incisions and more invasion. As for the other study (12), the authors reported the results of the procedure in four children, the outcomes were also good, despite the fact this series represented their initial experience
The overall number of cases of thymectomy in myasthenic patients has decreased significantly over the last 15 years. One of the reasons was that neurologists felt unease about sending patients to surgery without more sound evidence of benefit. However, this scenario is changing due to the randomized clinical trial comparing surgery with medical follow-up and demonstrated clinical benefit in the surgery arm (2). On top of that, both patients and neurologists have been more prone to accept the procedure if it is minimally invasive in opposition to a transsternal approach. Unfortunately, no further series was reported in Latin American literature.
Minimally invasive resection of thymic tumors was mentioned in early cohorts of patients undergoing resection of mediastinal tumors by VATS (8,10). Unfortunately, the authors did not go into details, but apparently all cases were small encapsulated thymomas. In the last decade, two case series reporting on management and outcomes of thymic tumors in Latin America were published, one in Brazil (16) and one in Chile (17). The Brazilian study included 26 patients with thymic malignancies operated on from 1986 until 2006. In no case was the VATS approach used (16). The Chilean study included 54 patients with thymic tumors (thymomas or thymic carcinomas) from 2000 to 2010, of which 47 underwent resection. Only 9 of the procedures started by VATS, and 3 of them were converted either to sternotomy or thoracotomy (17).
The BSTS has a national thoracic surgery database, which data collection started in July/2015. Five large academic institutions have been contributing to the database since its inception, and in 2017, 7 more have joined. Looking at the numbers, 43 patients were registered as having thymic tumors, 32 of them malignant (either thymomas or thymic carcinomas). Out of these 32 patients, 17 (53%) underwent VATS resections, no 30-day mortality in this group. The trend to MIS approaches becomes obvious with these numbers, now participants of the BSTS database are performing more than half of their thymic tumors resection by VATS, a huge contrast with the reality observed a decade ago. Even though, the current contributors are high-volume academic centers, they anticipate the change to come.
Personal approach
At University of Sao Paulo, we preferentially opt for MIS when treating patients with mediastinal tumors or myasthenia gravis. All patients are considered potential candidates; however, tumors larger than 8–10 cm and invasion of the heart or great vessels are usually excluded from the minimally invasive approach. Invasion of the lung, pericardium or chest wall is not a contra-indication for MIS in our group.
It’s been 10 years since we started our VATS program, so over these years most myasthenic patients and part of thymoma patients underwent 3-portal VATS resection in our institution. We prefer to perform the dissection through the right side and use CO2. The CO2 is very helpful, not only does it increase intrathoracic space, but it also helps with dissection and reduces blood oozing. In cases which the tumor is left-sided, we operate through the left.
A very important lesson learned is the fact that, when performing MIS, the whole process should be minimally invasive. More objectively, we had to get rid of epidurals, central lines, postoperative ICU, etc. This process, very well described in Cerfolio’s paper on lean thoracic surgery (18), brings great value to the care of the patient. And it is not easy to implement such a process, you have to include all parts in the discussion, anesthesiologists, nurses, neurologists and other medical staff, etc.
Two years ago, we started our robotic surgery program, and so far, we have performed 94 cases, 17 of them for mediastinal tumors or thymectomies for myasthenia. Even though this is an early experience, we could yet see the value of the robotic approach for such cases.
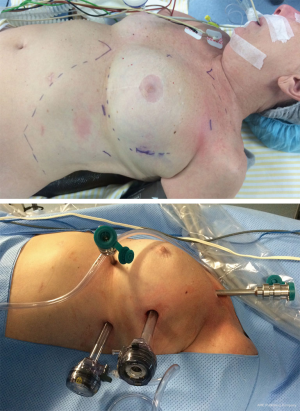
In our technique, we use three arms and, in some cases, a 4th portal for the assistant. Although we already had experience with the right-sided approach, we were convinced that the left-sided approach offers potential benefits, particularly in thymectomies for myasthenia. The main reason is the fact that in the left side the thymus is very close to the phrenic nerve and sometimes involves it, so the dissection of the left phrenic nerve can be more challenging. A left-sided approach makes it easier. Figure 1 shows the patient position and trocar sites. Figure 2 depicts a robotic resection of a thymoma performed in our institution.

Conclusions
Lack of publications makes it particularly difficult to analyze in more depth the current status of VATS in Latin America. Nonetheless, from the available information, we can conclude that MIS has been implemented slowly in the region and that costs and training are barriers for a faster dissemination of the method. Thymic surgery poses an additional challenge due to its rarity. Despite all that, MIS has an increasing role in the treatment of patients with myasthenia gravis and thymic tumors, and it already is the procedure of choice in half of those patients in large academic institutions.
Acknowledgements
None.
Footnote
Conflicts of Interest: Advisory board Johnson & Johnson and Medtronic, Educational grants H. Strattner/Intuitive.
References
- Friedant AJ, Handorf EA, Su S, et al. Minimally Invasive versus Open Thymectomy for Thymic Malignancies: Systematic Review and Meta-Analysis. J Thorac Oncol 2016;11:30-8. [Crossref] [PubMed]
- Wolfe GI, Kaminski HJ, Aban IB, et al. Randomized Trial of Thymectomy in Myasthenia Gravis. N Engl J Med 2016;375:511-22. [Crossref] [PubMed]
- Meyer DM, Herbert MA, Sobhani NC, et al. Comparative clinical outcomes of thymectomy for myasthenia gravis performed by extended transsternal and minimally invasive approaches. Ann Thorac Surg 2009;87:385-90; discussion 390-1. [Crossref] [PubMed]
- Qi K, Wang B, Wang B, et al. Video-assisted thoracoscopic surgery thymectomy versus open thymectomy in patients with myasthenia gravis: a meta-analysis. Acta Chir Belg 2016;116:282-8. [Crossref] [PubMed]
- Rodrigues OR, Losso LC, Ghefter MC, et al. Thoracoscopic surgery in Brazil. An overview. J Cardiovasc Surg (Torino) 1996;37:147-53. [PubMed]
- de Campos JR, Vargas FS, de Campos Werebe E, et al. Thoracoscopy talc poudrage: a 15-year experience. Chest 2001;119:801-6. [Crossref] [PubMed]
- Cirino LM, Milanez de Campos JR, Fernandez A, et al. Diagnosis and treatment of mediastinal tumors by thoracoscopy. Chest 2000;117:1787-92. [Crossref] [PubMed]
- Rosemberg NP, Schuler C, Delgiovo F, et al. Cisto broncogênico com abordagem videotoracoscópica. J Pneumol 2002;28:339-41. [Crossref]
- Barrenechea M, Korman L, Boglione M, et al. Cirugía torácica video asistida en los quistes broncogénicos. Rev. de Cir. Infantil 2002;12:173-5.
- Rodríguez AR, Sarria NC, Aja LT. Tumores de mediastino: informe sobre 29 pacientes. Rev Cubana Cir 2008;47:1-6.
- Saito EH, Higa C, Nunes RA, et al. Timectomia estendida por cirurgia torácica videoassistida e cervicotomia no tratamento da miastenia. J Pneumol 2003;29:273-9. [Crossref]
- Blanco A, Godoy J, Boye F, et al. Timectomía toracoscópica en pacientes pediátricos portadores de miastenia gravis. Rev. de Cir. Infantil 2004;14:77-79.
- Terra RM, Kazantzis T, Pinto-Filho DR, et al. Anatomic pulmonary resection by video-assisted thoracoscopy: the Brazilian experience (VATS Brazil study). J Bras Pneumol 2016;42:215-21. [Crossref] [PubMed]
- Sardenberg RA, Abadalla RZ, Abreu IR, et al. Robotic thymectomy for myasthenia gravis. J Bras Pneumol 2011;37:694-6. [Crossref] [PubMed]
- Terra RM, Araujo PH, Lauricella LL, et al. Robotic pulmonary lobectomy for lung cancer treatment: program implementation and initial experience. J Bras Pneumol 2016;42:185-90. [Crossref] [PubMed]
- Gross JL, Rosalino UA, Younes RN, et al. Characteristics associated with complete surgical resection of primary malignant mediastinal tumors. J Bras Pneumol 2009;35:832-8. [Crossref] [PubMed]
- González L R, Santolaya C R, Jadue T A, et al. Neoplasias epiteliales del timo: timoma y carcinoma tímico. Caracterización, tratamiento y variables asociadas a supervivencia. Rev. Chilena de Cirugía 2012;64:535-45. [Crossref]
- Cerfolio RJ, Steenwyk BL, Watson C, et al. Decreasing the Preincision Time for Pulmonary Lobectomy: The Process of Lean and Value Stream Mapping. Ann Thorac Surg 2016;101:1110-5. [Crossref] [PubMed]
- Terra RM. Resection of a Masaoka 1 thymoma by the means of thoracic robotic surgery. Asvide 2017;4:378. Available online: http://www.asvide.com/articles/1692
Cite this article as: Terra RM. Thymic minimally invasive surgery: state of the art across the world: Central-South America. J Vis Surg 2017;3:124.


