Uniportal video-assisted thoracoscopic surgery (VATS) technique is associated with decreased narcotic usage over traditional VATS lobectomy
Introduction
Video-assisted thoracoscopic surgery (VATS) has increasingly become the standard of care for many thoracic procedures. VATS allows for decreased post-operative hospitalization times and decreased peri-operative pain when compared to thoracotomy (1,2). Since it was first introduced in 1998, uniportal VATS technique has been consistently refined and is now used for a variety of procedures including sub-anatomic resections, lobectomies, and other major thoracic procedures (3-6). Though the popularity of uniportal VATS continues to grow, it is not without significant detraction and the debate on its efficacy and proper use continues (7). A recent meta-analysis demonstrated favorable outcomes when comparing multiport with uniportal VATS with regard to postoperative hospitalization, thoracostomy drainage duration, and morbidity (8).
Uniportal technique offers several potential benefits, one of which is decreased postoperative pain and resultant narcotic usage. In patients undergoing thoracoscopy for pneumothorax, uniportal technique was associated with decreased postoperative pain (9). Though a recent randomized study attempted to address this issue, there was considerable variation in methodology, particularly in the surgical technique used (10). Another observational study failed to show an appreciable difference in pain when comparing uniportal lobectomy to standard VATS technique, though the study was done as a non-inferiority report and included only 15 patients in the uniportal arm (11).
In addition, the previous studies have largely used visual analog scale (VAS) patient reporting as the collected metric regarding post-operative patient pain. While VAS data can be useful, it is a highly subjective marker of post-operative pain control, and subject to tremendous bias both from patients and clinicians. In addition, recent studies finding no change in VAS scores used a difference of two points to define significance, and clinical difference may exist below that threshold (12,13). Post-operative narcotic usage provides a much more objective and verifiable source of data regarding post-operative pain.
The purpose of this study was to determine the post-operative narcotic usage of consecutive patients undergoing anatomic lobectomy for presumed malignancy using both traditional multiport as well as uniportal technique.
Methods
This was a single center observational trial on prospectively collected data regarding all consecutive lobectomies for presumed malignancy by a single surgeon over the period of July 2013 to September 2015. The study was approved by the institutional review board of the University of Kansas Hospital. During the study period, the surgeon transitioned from multiport VATS to uniportal VATS.
Patients were excluded from the study if there was chronic opioid use, either prescribed or non-prescribed, before the operation. In addition, patients were excluded if they were under the age of 18 or if there was a thoracic epidural catheter placed prior to the operation. Patients that were converted from uniportal VATS to multiport VATS were included in the multiport group for the purposes of pain data analysis.
Data were collected regarding age, gender, American Society of Anesthesiologist (ASA) score, indication for operation, lymph node stations examined, hospital length of stay, length of post-operative thoracostomy, and any post-operative complications.
Operative technique and post-operative care
Multiport technique
Three incisions were used in standard fashion for visualization and mobilization of the pulmonary hilum. A 3–5 cm anterior utility incision located in approximately the 4th interspace directly over the hilum, a 5-mm camera port located in the 9th interspace in the midaxillary line, and a 1.5-cm incision in the 9th interspace in the posterior axillary line. The hilum was typically dissected anterior to posterior, and major vascular structures as well as the interlobar fissure were divided with Endo-GIA staplers (Covidien PLC, Dublin, Ireland). The specimen was removed in a bag from the anterior incision. A 28 F silastic thoracostomy tube was brought out through the inferior incision and secured. The incisions were closed in layers with absorbable sutures.
Uniportal technique
A single 4–5 cm incision was made in the 5th intercostal space anterior to the latissimus muscle. Serratus and intercostal fibers were divided. The soft tissues were retracted with sutures. A 5-mm 30-degree thoracoscope was inserted through this incision along with all working instruments. Similar to the multiport technique, the hilum was mobilized from anterior to posterior. Endo-GIA staplers were used to divide major vascular structures as well as the fissure. The same 28 F silastic thoracostomy was brought out through a muscular tunnel in the original incision, which was closed in layers with absorbable sutures.
All patients underwent intra-operative intercostal blocks at multiple levels as well as local infiltration at incision sites with 0.25% bupivacaine. All patients were initially prescribed a patient controlled analgesia (PCA) pump for pain control, which contained hydromorphone unless contraindicated. After diet was reinstituted, patients were transitioned to oral narcotic agents, most commonly immediate-release oxycodone, and this was continued until hospital discharge. Acetaminophen was routinely used as an adjunct for pain control, but other medications such as non-steroidal anti-inflammatory drugs were avoided. Narcotic medications were given per patient request, with acetaminophen administered on a round-the-clock schedule.
It has been our practice to remove chest drains when there is no evidence of air leak, and the character of the drainage is no longer sanguineous, with diminishing volumes of drainage over subsequent 8-hour intervals. Patients were discharged when mobile, eating a regular diet, and pain controlled with oral narcotics.
Statistical analysis
A database was maintained in Microsoft Excel (Microsoft Corporation, Redmond, WA, USA). Statistical analyses were performed using SPSS 20.0 (SPSS, Inc., Chicago, IL, USA). Continuous data were analyzed using Student’s t-test or the Mann-Whitney U-test where appropriate. Categorical data were analyzed using χ2 or Fisher’s exact test where appropriate. Significance was defined as P<0.05.
Results
Data were collected on 84 patients. Thirty-five patients underwent traditional multiport VATS and 49 patients underwent uniportal VATS. As outlined in Table 1, the two groups were well matched with regard to gender, age and indication for operative intervention. The median duration of stay was 3 days in both groups, though there was a trend toward earlier hospital discharge in the uniportal group. Both groups had a similar duration of indwelling thoracostomy, the multiport group with a median of 41 hours while the uniportal group had a median duration of 28 hours.
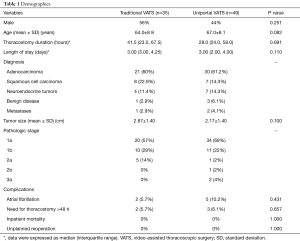
Full table
The groups had similar rates of postoperative complications, including atrial fibrillation and need for a thoracostomy greater than 48 hours. There were no unplanned reoperations in either group and there was no in-hospital or 30-day mortality in either group.
The uniportal group consumed significantly less narcotic medication at every time point when compared to the multiport group (Table 2). This difference was most pronounced during post-operative day 1, when the uniportal group consumed almost one half of the narcotic medication used by the multiport group. The daily differences resulted in a substantial decrease in the amount of narcotic consumed for the entire hospitalization in the multiport group.
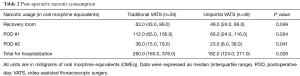
Full table
Discussion
This is the first study to demonstrate a significant decrease in the post-operative narcotic consumption when comparing multiport to uniportal VATS. Though other studies have failed to show this in the past, the standardized nature of the intraoperative and postoperative care of these patients is more rigorous in this current study. The use of post-operative narcotic consumption
This study has several limitations. The retrospective nature of the data lends themselves to inherent bias. However, this is somewhat mitigated by the standardized nature of the care the patients received. The low number of patients in each group could certainly be improved, though our sample size exceeds many similar retrospective studies on this topic. In addition, there was no randomization of patients, as this represents a series wherein practice patterns changed in favor of uniportal technique.
Uniportal VATS has thus far been shown to be safe and oncologically equivalent to traditional multiport VATS. Though there has been little randomized data, multiple case series have demonstrated a trend toward uniportal lobectomy as having benefit with regard to postoperative length of stay, thoracostomy duration, and morbidity.
In our study, the patients in the uniportal group consumed significantly less narcotic medication at all time points. In addition, there was no difference in other perioperative outcome measurement, though the patients in the uniportal group did have a trend toward earlier hospital discharge. Uniportal VATS lobectomy remains an exciting new development in the field of minimally invasive thoracic surgery, and one which may improve patient experience and outcome.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The study was approved by the institutional review board of the University of Kansas Hospital (Study00002406).
References
- Nagahiro I, Andou A, Aoe M, et al. Pulmonary function, postoperative pain, and serum cytokine level after lobectomy: a comparison of VATS and conventional procedure. Ann Thorac Surg 2001;72:362-5. [Crossref] [PubMed]
- Landreneau RJ, Hazelrigg SR, Mack MJ, et al. Postoperative pain-related morbidity: video-assisted thoracic surgery versus thoracotomy. Ann Thorac Surg 1993;56:1285-9. [Crossref] [PubMed]
- Migliore M. Initial History of Uniportal Video-Assisted Thoracoscopic Surgery. Ann Thorac Surg 2016;101:412-3. [Crossref] [PubMed]
- Rocco G, Martin-Ucar A, Passera E. Uniportal VATS wedge pulmonary resections. Ann Thorac Surg 2004;77:726-8. [Crossref] [PubMed]
- Gonzalez-Rivas D, Paradela M, Fernandez R, et al. Uniportal video-assisted thoracoscopic lobectomy: two years of experience. Ann Thorac Surg 2013;95:426-32. [Crossref] [PubMed]
- Migliore M, Deodato G. A single-trocar technique for minimally-invasive surgery of the chest. Surg Endosc 2001;15:899-901. [Crossref] [PubMed]
- Sihoe AD. Reasons not to perform uniportal VATS lobectomy. J Thorac Dis 2016;8:S333-43. [PubMed]
- Harris CG, James RS, Tian DH, et al. Systematic review and meta-analysis of uniportal versus multiportal video-assisted thoracoscopic lobectomy for lung cancer. Ann Cardiothorac Surg 2016;5:76-84. [Crossref] [PubMed]
- Jutley RS, Khalil MW, Rocco G. Uniportal vs standard three-port VATS technique for spontaneous pneumothorax: comparison of post-operative pain and residual paraesthesia. Eur J Cardiothorac Surg 2005;28:43-6. [Crossref] [PubMed]
- Perna V, Carvajal AF, Torrecilla JA, et al. Uniportal video-assisted thoracoscopic lobectomy versus other video-assisted thoracoscopic lobectomy techniques: a randomized study. Eur J Cardiothorac Surg 2016;50:411-5. [Crossref] [PubMed]
- McElnay PJ, Molyneux M, Krishnadas R, et al. Pain and recovery are comparable after either uniportal or multiport video-assisted thoracoscopic lobectomy: an observation study. Eur J Cardiothorac Surg 2015;47:912-5. [Crossref] [PubMed]
- Gonzalez-Rivas D, Damico TA, Jiang G, et al. Uniportal video-assisted thoracic surgery: a call for better evidence, not just more evidence. Eur J Cardiothorac Surg 2016;50:416-7. [Crossref] [PubMed]
- Kelly AM. The minimum clinically significant difference in visual analogue scale pain score does not differ with severity of pain. Emerg Med J 2001;18:205-7. [Crossref] [PubMed]
Cite this article as: Louis SG, Gibson WJ, King CL, Veeramachaneni NK. Uniportal video-assisted thoracoscopic surgery (VATS) technique is associated with decreased narcotic usage over traditional VATS lobectomy. J Vis Surg 2017;3:117.


