Subxiphoid approach for a combined right upper lobectomy and thymectomy through a single incision
Introduction
The thymic tumors are common in the 5th and 6th decade of the life without gender preference, near 10% of these are related to Myasthenia Gravis and other paraneoplastic syndromes (1). The treatment of these tumors is the complete surgical resection. The approach to this kind of tumors can be multiple from the Jarezki procedure to the minimally invasive surgery. A lot of reviews of these different approaches are published in the most important journals of thoracic surgery (2-7), Qi et al. support that the VATS had better outcomes of the patients against the open surgery (8). Ye et al. conclude that the Unilateral VATS Thymectomy is feasible, less invasive and safe than the transsternal thymectomy for Masaoka stage I and II (9). Suda et al. exposes that subxiphoid single port thymectomy is less invasive because the needed of painkillers, the days of hospitalization and the bleeding were lower than the VATS thymectomy group (10). Is for these and more research that support the subxiphoid approach for thymectomy and the flexibility to solve other lung pathologies in hands of surgeons with expertise in uniportal VATS by subxiphoid incision (11,12) that we present this case of right upper lobectomy and thymectomy by subxiphoid uniportal VATS in an anterior mediastinal mass and mass located in the right upper lobe.
Patient and workup
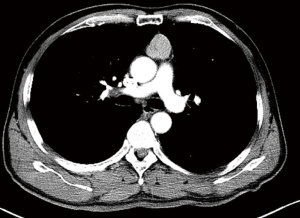
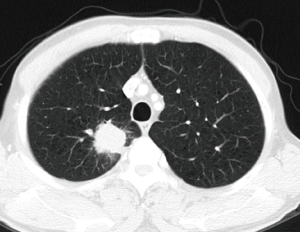
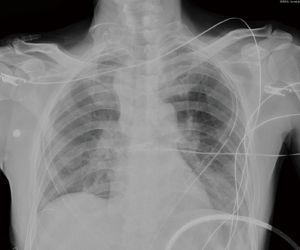
A 58-year-old male patient, without previous medical history or symptoms, which screening CT scan shows an anterior mediastinal mass of 3.1 cm × 4.1 cm (Figure 1), and a right upper lobe mass of 3.5 cm × 3.7 cm (Figure 2). The bronchoscopy was negative and no diagnosis was obtained before surgery. He was planned to perform both resections by the subxiphoid approach.
Pre-operative preparation
The operation was scheduled to perform both resections via uniportal VATS by subxiphoid technique. He was intubated with a double endotracheal tube, prophylaxis with cephalosporin, Central Venous Pressure line and Urinary catheters were inserted before the surgery.
Equipment performance card
Full HD thoracoscopic camera (Karl Stoz®), Uniportal Scanlan® VATS Instruments, Subxiphoid Uniportal VATS long adapted special instruments, Wound Protector (Changzhou Company LTd.), Endo GIA TM staplers (Covidien-Medtronic), Advanced Energy Device HARMONIC® (Ethicon).
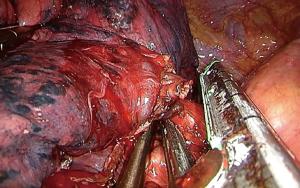
Procedure (Figure 3)

Under general anesthesia, insertion of CVP line and urinary catheter, the patient was positioned in a left lateral position with 60° of inclination, and a 4 cm midline median incision below the sternocostal triangle was performed. The lobectomy was started with the dissection of the pleura, identification and dissection of the right upper lobe vein and the anterior and apical arteries that were divided with EndoGIA® Vascular Staplers. The next step was the division of the anterior part of the fissure with EndoGIA® green stapler. The right upper lobe bronchus was divided with a EndoGIA® green stapler (Figure 4) and the Posterior ascending arteries were exposed and divided with Vascular Clips (GRENA®) by using a 45 specific applier. The right upper lobe was extracted in endobag trough the incision. The lymphadenectomy was performed in the station 2, 4R and 7.
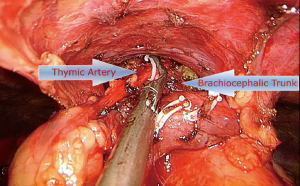
Both the right and left pleura were opened and the dissection of the fat pads in the epiphrenic and pericardial area were performed by using a long curved specific electrocautery and HARMONIC® scalpel, formerly, both lobes of the thymus were dissected in cephalic direction to the confluence of brachiocephalic venous trunks including both horns. The Thymic vessels were dissected, exposed a clipped with Vascular polymer Clips. In this case we found three thymic veins tributaries of the left brachiocephalic venous trunk and one thymic artery branch of the right brachiocephalic arterial trunk who is uncommon anatomical variant (Figure 5). The thymectomy was concluded and the complete gland with the perithymic tissue was removed en bloc. The hemostasis was verified and two chest drains of 28 Fr were placed through the same incision. The estimated blood loss during the surgery was 100 mL and the total surgical time was 160 minutes (Figure 6).
Post-operative management
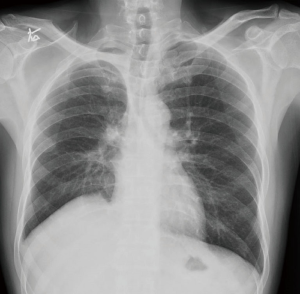
The post-operative course of the patient was successful without complications. The management of the pain was with patients controlled analgesia (PCA) and oxycodone medication. The post-operative X-ray shows complete expanded lungs without pneumothorax or hemothorax (Figure 6). The chest tubes were removed in the POD N°5, the X-ray after the removal of the tubes was normal (Figure 7) and the patient was discharged in the POD N°10.
The paraffin biopsy results were in the mass of the right upper lobe: adenocarcinoma pT2aN0M0 (stage IB) and the mediastinal tumor: thymoma.
Tips, tricks and pitfalls
- Open the pleura of both sides will provide a better view and more space for the dissection of the thymus and the perithymic tissue.
- Perform the Thymectomy from caudal to cranial and both sides at the same time until the confluence of the Brachiocephalic Venous Trunks gives a facility to recognize the thymic vessels and the different anatomical variants.
- Taking into account the anatomical variants of the thymus irrigation is important to perform a careful dissection in order to avoid intraoperative bleeding, which could be really difficult to control by a subxiphoid approach.
- The Subxiphoid Uniportal VATS approach provides to an expert thoracic surgeon the flexibility to performed combined surgeries through the same incision.
Acknowledgements
None.
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient for publication of this manuscript and any accompanying images.
References
- Sugarbaker D, Bueno R, Colson Y, et al. United States of America, Adult Chest Surgery, Second edition. Mac Graw Hill Education, 2015.
- Wu L, Lin L, Liu M, et al. Subxiphoid uniportal thoracoscopic extended thymectomy. J Thorac Dis 2015;7:1658-60. [PubMed]
- Fiorelli A, Mazzella A, Cascone R, et al. Bilateral thoracoscopic extended thymectomy versus sternotomy. Asian Cardiovasc Thorac Ann 2016;24:555-61. [Crossref] [PubMed]
- Suda T, Kaneda S, Hachimaru A, et al. Thymectomy via a subxiphoid approach: single-port and robot-assisted. J Thorac Dis 2016;8:S265-71. [PubMed]
- Zhao J, Wang J, Zhao Z, et al. Subxiphoid and subcostal arch thoracoscopic extended thymectomy: a safe and feasible minimally invasive procedure for selective stage III thymomas. J Thorac Dis 2016;8:S258-64. [PubMed]
- Yano M, Moriyama S, Haneda H, et al. Thymectomy using the subxiphoid approach. J Thorac Cardiovasc Surg 2016;152:278-9. [Crossref] [PubMed]
- Suda T. Single-port thymectomy using a subxiphoid approach-surgical technique. Ann Cardiothorac Surg 2016;5:56-8. [PubMed]
- Qi K, Wang B, Wang B, et al. Video-assisted thoracoscopic surgery thymectomy versus open thymectomy in patients with myasthenia gravis: a meta-analysis. Acta Chir Belg 2016;116:282-8. [Crossref] [PubMed]
- Ye B, Tantai JC, Ge XX, et al. Surgical techniques for early-stage thymoma: video-assisted thoracoscopic thymectomy versus transsternal thymectomy. J Thorac Cardiovasc Surg 2014;147:1599-603. [Crossref] [PubMed]
- Suda T, Hachimaru A, Tochii D, et al. Video-assisted thoracoscopic thymectomy versus subxiphoid single-port thymectomy: initial results†. Eur J Cardiothorac Surg 2016;49 Suppl 1:i54-8. [PubMed]
- Hernandez-Arenas LA, Lin L, Yang Y, et al. Initial experience in uniportal subxiphoid video-assisted thoracoscopic surgery for major lung resections. Eur J Cardiothorac Surg 2016;50:1060-6. [Crossref] [PubMed]
- Gonzalez-Rivas D, Yang Y, Lei J, et al. Subxiphoid uniportal video-assisted thoracoscopic middle lobectomy and anterior anatomic segmentectomy (S3). J Thorac Dis 2016;8:540-3. [Crossref] [PubMed]
- Argueta AJ, Cañas SR, Abu Akar F, et al. Subxiphoid uniportal VATS: right upper lobectomy and thymectomy. Asvide 2017;4:322. Available online: http://www.asvide.com/articles/1634
Cite this article as: Argueta AJ, Cañas SR, Abu Akar F, Gonzalez-Rivas D. Subxiphoid approach for a combined right upper lobectomy and thymectomy through a single incision. J Vis Surg 2017;3:101.