Minimally invasive esophagectomy: Chinese experiences
Esophageal cancer is one of the most popular malignant tumors in China, which has high morbidity and mortality rate (1,2). Squamous cell carcinoma is much more frequently observed in Chinese esophageal cancer patients than adenocarcinoma. Depending on the location of tumor, Ivor Lewis or McKeown surgical approach is adopted for resectable esophageal cancer (3,4). These approaches are widely accepted with the advantages of mediastinal lymphadenectomy, low perioperative morbidity (5). The 5-year survival rate of esophageal cancer has been greatly improved to almost 40% through the surgical progress, early screening, and multidisciplinary treatment in recent decades (6). However, the perioperative morbidity and mortality remain unsolved problem as a result of enlarged lymphadenectomy, thorough en bloc dissection, and so on (7,8). In open surgery, post-operation pain might last a very long time and the perioperative morbidity including cardiopulmonary complications could reach as high as 30% (9,10).
Minimally invasive esophagectomy (MIE) has gradually become a standard surgical approach for esophageal cancer in recent years. It was first report by Dr. Cuschieri in 1993 (11) and implemented by many thoracic surgeons, such as Dr. Luketich. In 2003, a report of 222 cases of MIE was published (12), while another report of more than 1,000 cases of MIE was published in 2012 (13). A randomized multicenter clinical study by Biere et al. provided strong evidence of the short-term benefits of MIE for patients (14). Nowadays, MIE has been widely accepted in Japan, Europe, and America.
Esophageal cancer is one of the most common cancers in China (1,2). The incidence and morbidity of esophageal cancer remains very high in China nowadays. Early prevention and treatment for esophageal cancer is important and still a major task. MIE has emerged as effective alternative approach for open surgery in recent decades in China. Most of Chinese advanced esophageal centers, including Zhongshan hospital of Fudan University, The First affiliated Hospital of Fujian Medical School, Cancer Hospital of Chinese Academy of Medical Sciences, have adopted MIE as routine surgical approach for resectable patients. Our center performed the first case of MIE in China in 2004. From January 2004 to December 2015, we have successfully performed more than 1,300 cases of MIE. Since most esophageal cancer is squamous cell carcinoma and locates in the middle of esophagus, McKeown is preferred in our center.
Patients and surgical procedure
Patients
According to the NCCN guideline and Chinese Esophageal Cancer guideline, resectable patients in China are defined as follows:
- Age <80 y;
- T1–T3, without metastasis;
- without severe complications;
- without other malignant tumor;
- ECOG score 0–1.
Anesthesia and position
Combined general-epidural anesthesia and a single-lumen endotracheal tube are adopted before surgery. Commonly, we place patient in the left lateral prone position, but not the left lateral decubitus position or the prone position, which are common in western countries.
The thoracic port design and artificial pneumothorax
The observation port is selected in the 7th intercostal spaces of the posterior axillary line. Artificial pneumothorax is then set up through the trocar in the observation port, and the CO2 pressure is controlled between 8−10 mmHg. Other trocars are located: the 3rd intercostal spaces of the mid-axillary line, the 9th intercostal spaces of the subscapular line, and the 6th intercostal spaces of the subscapular line (Figure 1).
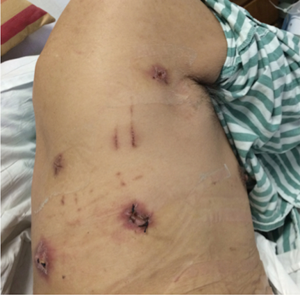
Thoracoscopic, laparoscopic and cervical procedure
The procedure of thoracic surgery is performed in standard manner as open surgery (Figure 2). (I) Opening the mediastinal pleura of the supra-azygos area, and cleaning the right para-laryngeal recurrent nerve lymph nodes; (II) clipping and cutting the arch of the azygos; (III) opening the mediastinal pleura of the sub-azygos area, and circumferential mobilization of the middle and lower part of esophagus; (IV) lifting the esophagus through a silk thread and cleaning the left para-laryngeal recurrent nerve lymph nodes; (V) total mobilization of the esophagus.

The procedure of abdominal and cervical part is performed as described by other surgeons (16). Patient is placed in supine position. Gastric mobilization is performed under laparoscopy (Figure 3). Then, a left cervical incision is made and the cervical esophagus is dissected and transected. A 4 cm middle abdominal incision is made, and the stomach and esophagus are retracted from this incision. A linear cutting stapler is used to make gastric tube. The anastomosis between gastric tube and cervical esophagus is performed through the cervical incision with circular anastomat.

Discussion
Esophageal cancer is one of the four most common cancers in China, with high mortality. The pathological type of esophageal cancer in China is mostly squamous cell carcinoma, which is quite different from western countries. Treatment for esophageal cancer includes surgical therapy, radiotherapy, chemotherapy, and combined therapy. Open surgery was once the only choice for resectable patients before the emergence of MIE. MIE was first performed by Cuschieri in 1993 (11), and then introduced to China in 1994. As one of the largest esophageal cancer center in China, our center performed the first case of MIE in China in 1994, and the total number of our MIE cases has exceeded 1,300.
MIE has gradually become the standard surgical procedure for esophageal cancer because of its advantages in perioperative morbidity and mortality. In 2012, Lancet has published the report of a randomized controlled multicenter clinical trial in Europe, which supports that MIE reduces cardiopulmonary complications. However, the sample of this study is not large enough (14). Dr. Luketich also studied this topic with almost 1,000 cases (13). However, it’s still necessary to re-evaluate the benefits of MIE in China, because of the different pathological type and surgical approach. Experiences of our center support that MIE has better short-term outcome than open surgery. The incidence of perioperative complications is significantly reduced. However, data from our center shows the anastomotic leak incident does not vary with the operation approach. And the overall survival rate is also not influence by surgical approach. Similar results have been reported by other Chinese esophageal cancer center (18-20).
Two positions of thoracic surgery in MIE are commonly adopted by surgeons from western countries, including the left lateral decubitus position and the prone position. But in China, the lateral prone position is more popular (20). The left lateral decubitus position was firstly adopted in MIE, because of the anatomical similarity as open surgery. The prone position was then introduced in to MIE because of its clear exposure of mediastinal organs and structures. However, one main disadvantage of the prone position is that changing position is required in case of emergency. The lateral prone position with artificial pneumothorax not only provides clear exposure of surgical area, but also avoids the position change in case of emergency. At present, this position has also been accepted by many centers in the world.
Lymph node dissection is an important part of MIE surgery. 3FLD esophagectomy is not a routine surgery in China due to its high invasiveness. In the 2FLD esophagectomy, MIE always has a better lymph node dissection than open surgery, because of its enlarged view of surgical area by thoracoscopy and laparoscopy. The left para-laryngeal recurrent nerve lymph nodes are difficult to dissect under thoracoscopy through the surgical approach from right chest. Esophageal suspension is a good manner for the exposure and dissection of the left para-laryngeal recurrent nerve lymph nodes. The esophagus is lifted through a silk thread in order to pull the left-laryngeal recurrent nerve and its nearby structures into right chest. The incidence of nerve injury is reduced and the dissected lymph node number is increased with esophageal suspension in this way.
Since its first introduction to China in 1994, MIE has become widely accepted and developed in the past decades in China. Most advanced esophageal centers performed hundreds of MIE and accumulated abundant experiences. The benefits of short term outcomes of MIE are confirmed by studies in China. However, the long term survival and the anastomosis leakage results are still uncertain and need more research. Generally, MIE is safe, feasible and suitable surgical approach for resectable esophageal cancer.
Acknowledgements
Funding: This study was supported by the National Nature Science Foundation of China (Grant Nos. 81500568, 81370587).
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The study was approved by ethics committee of Zhongshan Hospital (No. B2013-115) and written informed consent was obtained from all patients.
References
- Zeng H, Zheng R, Zhang S, et al. Esophageal cancer statistics in China, 2011: Estimates based on 177 cancer registries. Thorac Cancer 2016;7:232-7. [Crossref] [PubMed]
- Chen W, Zheng R, Baade PD, et al. Cancer statistics in China, 2015. CA Cancer J Clin 2016;66:115-32. [Crossref] [PubMed]
- Chadwick G, Riley S, Hardwick RH, et al. Population-based cohort study of the management and survival of patients with early-stage oesophageal adenocarcinoma in England. Br J Surg 2016;103:544-52. [Crossref] [PubMed]
- Little AG, Lerut AE, Harpole DH, et al. The Society of Thoracic Surgeons practice guidelines on the role of multimodality treatment for cancer of the esophagus and gastroesophageal junction. Ann Thorac Surg 2014;98:1880-5. [Crossref] [PubMed]
- Ando N, Ozawa S, Kitagawa Y, et al. Improvement in the results of surgical treatment of advanced squamous esophageal carcinoma during 15 consecutive years. Ann Surg 2000;232:225-32. [Crossref] [PubMed]
- Shapiro J, van Lanschot JJ, Hulshof MC, et al. Neoadjuvant chemoradiotherapy plus surgery versus surgery alone for oesophageal or junctional cancer (CROSS): long-term results of a randomised controlled trial. Lancet Oncol 2015;16:1090-8. [Crossref] [PubMed]
- Jafari MD, Halabi WJ, Smith BR, et al. A decade analysis of trends and outcomes of partial versus total esophagectomy in the United States. Ann Surg 2013;258:450-8. [Crossref] [PubMed]
- Seely AJ, Ivanovic J, Threader J, et al. Systematic classification of morbidity and mortality after thoracic surgery. Ann Thorac Surg 2010;90:936-42; discussion 942. [Crossref] [PubMed]
- van der Sluis PC, Verhage RJ, van der Horst S, et al. A new clinical scoring system to define pneumonia following esophagectomy for cancer. Dig Surg 2014;31:108-16. [Crossref] [PubMed]
- Yoshida N, Watanabe M, Baba Y, et al. Risk factors for pulmonary complications after esophagectomy for esophageal cancer. Surg Today 2014;44:526-32. [Crossref] [PubMed]
- Cuschieri A. Endoscopic subtotal oesophagectomy for cancer using the right thoracoscopic approach. Surg Oncol 1993;2 Suppl 1:3-11. [Crossref] [PubMed]
- Luketich JD, Alvelo-Rivera M, Buenaventura PO, et al. Minimally invasive esophagectomy: outcomes in 222 patients. Ann Surg 2003;238:486-94; discussion 494-5. [PubMed]
- Luketich JD, Pennathur A, Awais O, et al. Outcomes after minimally invasive esophagectomy: review of over 1000 patients. Ann Surg 2012;256:95-103. [Crossref] [PubMed]
- Biere SS, van Berge Henegouwen MI, Maas KW, et al. Minimally invasive versus open oesophagectomy for patients with oesophageal cancer: a multicentre, open-label, randomised controlled trial. Lancet 2012;379:1887-92. [Crossref] [PubMed]
- Lin M, Shen Y, Tan L, et al. Thoracoscopic procedures. The mobilization of the esophagus and the lymph node dissection are performed under thoracoscopy. Asvide 2016;3:317. Available online: http://www.asvide.com/articles/1074
- Palanivelu C, Prakash A, Senthilkumar R, et al. Minimally invasive esophagectomy: thoracoscopic mobilization of the esophagus and mediastinal lymphadenectomy in prone position--experience of 130 patients. J Am Coll Surg 2006;203:7-16. [Crossref] [PubMed]
- Lin M, Shen Y, Tan L, et al. Laparoscopic procedures. The mobilization of the stomach is performed under laparoscopy. Asvide 2016;3:318. Available online: http://www.asvide.com/articles/1075
- Zhu C, Jin K. Minimally invasive esophagectomy for esophageal cancer in the People's Republic of China: an overview. Onco Targets Ther 2013;6:119-24. [PubMed]
- Mu J, Yuan Z, Zhang B, et al. Comparative study of minimally invasive versus open esophagectomy for esophageal cancer in a single cancer center. Chin Med J (Engl) 2014;127:747-52. [PubMed]
- Li X, Lai FC, Qiu ML, et al. Minimally Invasive Esophagectomy in the Lateral-prone Position: Experience of 226 Cases. Surg Laparosc Endosc Percutan Tech 2016;26:60-5. [Crossref] [PubMed]
Cite this article as: Lin M, Shen Y, Feng M, Tan L. Minimally invasive esophagectomy: Chinese experiences. J Vis Surg 2016;2:134.


