Delta-shaped Billroth-I anastomosis in totally laparoscopic distal gastrectomy with D2 lymph node dissection for gastric cancer
Introduction
Gastroduodenostomy (Billroth-I anastomosis), a preferable method of gastrointestinal tract reconstruction for distal gastrectomy, is usually applied in open surgery. We herein describe our experience of finishing it under laparoscopy, which is widely accepted as delta-shaped Billroth-I anastomosis.
Methods
Patient selection and workup
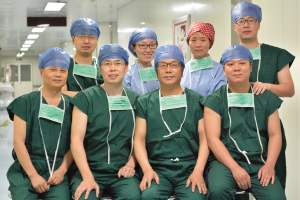
Laparoscopic delta-shaped Billroth-I anastomosis is recommended for the selected patients with small-diameter early-stage gastric cancer at gastric angle. The present video (Figure 1) by my surgical team (Figure 2) recorded the operation of a 61-year-old woman with body mass index of 23.5 kg/m2. She suffered from upper abdominal pain for 2 months and then underwent gastroscopy, by which a superficial ulcer of approximately 1 cm in diameter at gastric angle was discovered. Endoscopic ultrasound showed that the lesion was confined to the submucosa and suspected malignancy. The diagnosis of poorly-to-moderately differentiated adenocarcinoma was confirmed by later biopsy and histological test. There is no positive finding in physical exam, assay of serum tumor markers, chest X-ray and abdominal CT. The tumor stage was assessed to be cT1N0M0. She underwent delta-shaped Billroth-I anastomosis after laparoscopic distal gastrectomy with D2 lymph node dissection. The work was approved by the ethnical committee of our hospital, and the patient was informed before surgery.

Gastroscopy during the operation
Since the lesion only invaded the submucosa of gastric wall and was invisible on the serosa layer by laparoscopy, gastroscopy was performed to confirm its exact location during the operation.
Postoperative management
Prophylactic antibiotic treatment was given for 48 hours after surgery. A liquid diet was allowed on postoperative day 4 and continued for 3 days, followed by semi-liquids, till she was discharged on postoperative day 11.
Results
It took about 120 min to finish the operation with blood loss of about 50 mL. The pathology report was that poorly-to-moderately differentiated adenocarcinoma of 1.0 cm × 1.2 cm at the lesser curvature of stomach invaded submucosa and metastasized to 1 of 31 paragastric lymph nodes. The tumor stage was pT1N1M0. The patient recovered well and was prescribed chemotherapeutic regimens of XELOX. She had been well-tolerated for three courses of chemotherapy.
Discussion
Billroth-I anastomosis following distal gastrectomy has the physiological advantage of allowing food to pass through the duodenum. So it has been widely used as a standard reconstruction method. The anastomosis is usually completed by hand-sewing or circular stapling, either of which, however, is hard to be duplicated in laparoscopic surgery. The demand of designing an easy-to-use method eventually generates the new method of intracorporeal gastroduodenostomy, namely delta-shaped Billroth-I anastomosis, in which only endoscopic linear staplers are used (2).
The anastomosis is created between the posterior walls of the stomach and the duodenal bulb. The duodenum is first transected near the pylorus, with the duodenum bulb of 2–3 cm long left, by linear stapling from the posterior to the anterior wall. The stomach is transected by one or two linear staplers as usual, from the greater to the lesser curvature. Gastroscopy is recommended to ensure the margins of the resected distal stomach not too close to the tumor before the duodenum and stomach are transected. Conversely, if the remnant stomach is too small or if the duodenal bulb is too short, the anastomosis may be under unfavorable tension, and consequently at high risk of anastomotic leakage. Therefore, the patients who undergo the surgery should be carefully selected to meet the following criteria: early-stage gastric cancer, small size of tumor, and preferably tumor at gastric angle.
After the distal stomach is removed, small incisions, each of which is merely to allow inserting one limb of a 60 mm linear stapler, are made at the cutting edge of gastric wall near the greater curvature and at the cutting edge of duodenal posterior wall, respectively. If the incisions are too long, they may be too hard to close later on. The posterior walls of the stomach and the duodenum are approximated and anastomosed with a linear stapler. The stapling line is then inspected through the common stab incision for any defects. In the end, the common stab incision is closed at the direction vertical to the cutting edge of stomach by a linear stapler. The procedure has evolved by extending the last stapling line to the anterior wall of duodenal bulb, that is, transecting duodenal bulb again (3). The initial cutting edge of duodenal bulb is completely resected, which eliminates the intersection of duodenal cutting edge and theoretically lowers the risk of anastomosis-related complication. The anastomosis appears as an inverted T-shape.
Conclusions
The delta-shaped Billroth-I anastomosis is a safe and feasible laparoscopic reconstruction method for early-stage distal gastric cancer. It has the advantage of minimal invasiveness, good operative views and short operative time. Satisfactory outcomes are guaranteed if we know its technical details.
Acknowledgements
Funding: The work is supported by Zhejiang Province Public Technology Applied Research Project (No. 2014C33236) and project of medicine and health science and technology of Zhejiang province (No. 2014KYB192).
Footnote
Conflicts of Interest: The authors have no conflicts of interest to declare.
Ethical Statement: The work was approved by the ethnical committee of our hospital. Written informed consent was obtained from the patient. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
References
- Zhang J, Ying RC, Wei W, et al. Delta-shaped Billroth-I anastomosis following laparoscopic distal gastrectomy was performed. Asvide 2016;3:221. Available online: http://www.asvide.com/articles/980
- Kanaya S, Gomi T, Momoi H, et al. Delta-shaped anastomosis in totally laparoscopic Billroth I gastrectomy: new technique of intraabdominal gastroduodenostomy. J Am Coll Surg 2002;195:284-7. [Crossref] [PubMed]
- Huang C, Lin M, Chen Q, et al. A modified delta-shaped gastroduodenostomy in totally laparoscopic distal gastrectomy for gastric cancer: a safe and feasible technique. PLoS One 2014;9:e102736. [Crossref] [PubMed]
Cite this article as: Zhang J, Ying RC, Wei W, Zhu AK, Yin G. Delta-shaped Billroth-I anastomosis in totally laparoscopic distal gastrectomy with D2 lymph node dissection for gastric cancer. J Vis Surg 2016;2:100.


