Combining all forces: abdominoperineal resection in an obese male
IntroductionOther Section
- Introduction
- Patient selection and workup
- Pre-operative preparation
- Equipment preference card
- Procedure (Figure 2)
- Post-operative management
- Tips, tricks, and pitfalls
- Conclusions
- Acknowledgements
- Footnote
- References
Open rectal cancer surgery is associated with longer hospitalization and increased morbidity (1). The laparoscopic approach to rectal cancer is difficult secondary to the restricted degrees of freedom of current instruments making precise dissection difficult and time consuming (2). As colorectal procedures often involve multiple abdominal quadrants, the robot with its limited range of arm movements makes mobilization outside the deep pelvis difficult (2). Augmenting the challenge are viscerally obese patients who have a significantly higher conversion rate to open procedures translating to increased morbidity and longer hospital stay (3). Patients undergoing major colorectal surgery have morbidity and mortality rates of 36% and 14%, respectively (3,4). The stability of platform, retraction, high definition optics and improved dexterity of robot instrumentation offers advantages in dissection of a bulky mesorectum within a narrow pelvis. Although there are disadvantages that exist with each technique, unique aspects of each approach can be applied to a difficult dissection, such as a long and narrow pelvis in obese patients.
A hybrid technique that includes laparoscopic colon mobilization and robotic rectal dissection has been widely adopted showing safety and feasibility with acceptable pathologic and oncological outcomes (2,5). In order to highlight the advantages applied to a difficult dissection, we present the components of the hybrid approach, inclusive of hand assistance, to an abdominoperineal resection in an obese male.
Patient selection and workupOther Section
- Introduction
- Patient selection and workup
- Pre-operative preparation
- Equipment preference card
- Procedure (Figure 2)
- Post-operative management
- Tips, tricks, and pitfalls
- Conclusions
- Acknowledgements
- Footnote
- References
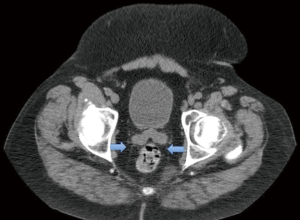
The patient was a 58-year-old male, with a BMI of 36 kg/m2, diagnosed with a squamous cell carcinoma of the anal canal 5 cm in size. Despite undergoing chemoradiation with the Nigro protocol, the tumor recurred. Inguinal lymph nodes were not palpable. Secondary to persistent disease localized to the pelvis, salvage therapy was offered in the form of an abdominoperineal resection. A hybrid, multi-modal approach was ideally suited for this deep pelvic tumor in a tall, obese male with a narrow pelvis (Figure 1).
Pre-operative preparationOther Section
- Introduction
- Patient selection and workup
- Pre-operative preparation
- Equipment preference card
- Procedure (Figure 2)
- Post-operative management
- Tips, tricks, and pitfalls
- Conclusions
- Acknowledgements
- Footnote
- References
Pre-operatively a complete blood count, electrolytes, liver and renal functions were obtained. Bowel preparation was administer one day before the procedure, and the patient was instructed to fast for at least 6 hours pre-operatively. Prophylactic antibiotics were administered 30 minutes before incision. Appropriate consent per our institutional protocol inclusive of multi-media content was obtained.
Equipment preference cardOther Section
- Introduction
- Patient selection and workup
- Pre-operative preparation
- Equipment preference card
- Procedure (Figure 2)
- Post-operative management
- Tips, tricks, and pitfalls
- Conclusions
- Acknowledgements
- Footnote
- References
- DaVinci surgical system (Intuitive Surgical Inc., Sunnyvale, CA, USA);
- Laparoscopic setup;
- Exploratory laparotomy tray (on standby);
- 8 mm robotic trocars ×3;
- Cadiere forceps (bipolar attachment);
- Monopolar electrocautery hook;
- Atraumatic bowel grasper;
- 0° 12 mm laparoscopic camera;
- 12 mm trocar.
Procedure (Figure 2)Other Section
- Introduction
- Patient selection and workup
- Pre-operative preparation
- Equipment preference card
- Procedure (Figure 2)
- Post-operative management
- Tips, tricks, and pitfalls
- Conclusions
- Acknowledgements
- Footnote
- References

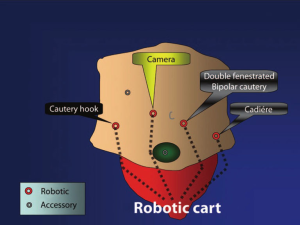
After induction of general anesthesia, a urinary catheter, oro-gastric tube, and appropriate intravenous access were placed. The patient was positioned in modified lithotomy and the abdomen was prepared and draped in the standard sterile fashion. After pneumoperitoneum was established, additional laparoscopic ports were placed. Diagnostic laparoscopy revealed that exposure to the inferior mesenteric artery (IMA) was difficult due to excessive visceral fat. Further exposure demonstrated a bulky mesorectum within a restricted working space. This represented an ideal scenario for the utilization of the robot as part of the multi-modal approach. A hand assist port was placed through a Pfannenstiel incision to help with the dissection of the mesentery and to facilitate exposure of the IMA. Tactile feedback through the handport allowed us to perform a fully controlled, oncologic dissection with a high ligation of the vascular pedicle without interference from the small bowel. Retroperitoneal dissection in the left lower quadrant was performed keeping the Toldt’s fascia intact for the preservation of the IMA and superior hypogastric plexuses as well as ureters. After the mobilization of the sigmoid, it was exteriorized through the hand port and transected with a linear stapler. The thick sigmoid mesentery was divided intracorporeally resulting in the complete isolation of the rectosigmoid stump in preparation of total mesorectal excision (TME). The robot cart was docked between the patient’s legs and two additional ports were added to the left side of the abdomen. Five actively working instruments were used for the TME (Figure 3).
The rectal stump was retracted anteriorly and posterior dissection commenced at the sacral promontory. The hypogastric nerve plane was identified and the nerves were preserved. The ‘holy’ plane was entered through the incised pre-hypogastric nerve fascia. The patient’s body habitus and the edema from prior radiation made maneuvering in the holy plane difficult. Likewise, anterior dissection was expected to be challenging in this patient. The rectal stump was retracted posteriorly and a proper plane was developed along the posterior surface of Denonvillier’s fascia preserving the autonomic nerves while leaving the seminal vesicles and prostate intact. Dissection was carefully undertaken in a gradual, circumferential fashion. Two main features of the robotic device could be generally appreciated at that junction: (I) the stability of the platform; and (II) the precision of dissection in that environment. The dissection was extended to the lateral aspect of the mesorectum exposing its deep lateral aspects. Due to the technical difficulties encountered in this challenging patient, a robotic intra-abdominal levator transection (RILT) was not possible. Therefore, we decided to proceed with a perineal resection of the levators. After ensuring careful hemostasis, the abdomen was desufflated, the port sites were closed, and a colostomy was matured.
The patient was placed in the prone jackknife position, and a perineal incision that included a coccygectomy was performed to facilitate the cylindrical transection of the levators. Dissection was deepened to the peritoneum and eccentrically directed to the left side around the tumor. After identification, the levators were transected at the posterior and lateral aspects. The specimen was then exteriorized to complete the anterior dissection and it was removed. An omental pedicle flap was created to fill the empty pelvic space. The final specimen revealed an intact cylindrical mesorectum with the levators and coccyx attached. After careful inspection of the surgical site, a drain was placed, and the wound was closed.
Post-operative managementOther Section
- Introduction
- Patient selection and workup
- Pre-operative preparation
- Equipment preference card
- Procedure (Figure 2)
- Post-operative management
- Tips, tricks, and pitfalls
- Conclusions
- Acknowledgements
- Footnote
- References
The patient was managed according to established post operative supportive protocols including the administration of appropriate pain management. A clear liquid diet was administered once evidence of bowel function was demonstrated through the stoma. The patient was discharged once his pain was well controlled on oral analgesics and he was able to ambulate safely and tolerate a soft diet. The patient was followed up post-operatively as per National Comprehensive Cancer Network Guidelines (NCCN).
Tips, tricks, and pitfallsOther Section
- Introduction
- Patient selection and workup
- Pre-operative preparation
- Equipment preference card
- Procedure (Figure 2)
- Post-operative management
- Tips, tricks, and pitfalls
- Conclusions
- Acknowledgements
- Footnote
- References
- The management of rectal cancer can be complex and requires a multidisciplinary clinical approach;
- Open rectal cancer surgery is associated with longer hospitalization and increased morbidity;
- The laparoscopic approach to rectal cancer in obese patients is plagued with difficulty secondary to the restricted degrees of freedom of current instruments;
- The robot with limited range of arm movement makes four quadrant intracorporeal maneuvering difficult;
- Obesity is a risk factor for post-operative morbidity in patients undergoing colorectal surgery and can augment the difficulty of visceral and pelvic dissection;
- A multi-modal application (hand assist, laparoscopic, and robotic) for specific operative scenarios can be helpful to achieve an optimal outcome;
- A robotic platform could potentially facilitate intra-abdominal levator transection (RILT).
ConclusionsOther Section
- Introduction
- Patient selection and workup
- Pre-operative preparation
- Equipment preference card
- Procedure (Figure 2)
- Post-operative management
- Tips, tricks, and pitfalls
- Conclusions
- Acknowledgements
- Footnote
- References
We have demonstrated a case where a multi-modal approach can be useful in achieving a minimally invasive abdominoperineal resection. This was particularly useful in the narrow pelvic space of an obese male. However, further studies are required to prove the efficacy of this approach.
AcknowledgementsOther Section
- Introduction
- Patient selection and workup
- Pre-operative preparation
- Equipment preference card
- Procedure (Figure 2)
- Post-operative management
- Tips, tricks, and pitfalls
- Conclusions
- Acknowledgements
- Footnote
- References
None.
FootnoteOther Section
- Introduction
- Patient selection and workup
- Pre-operative preparation
- Equipment preference card
- Procedure (Figure 2)
- Post-operative management
- Tips, tricks, and pitfalls
- Conclusions
- Acknowledgements
- Footnote
- References
Conflicts of Interest: The authors have no conflicts of interest to declare.
Informed Consent: Written informed consent was obtained from the patient for publication. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
ReferencesOther Section
- Introduction
- Patient selection and workup
- Pre-operative preparation
- Equipment preference card
- Procedure (Figure 2)
- Post-operative management
- Tips, tricks, and pitfalls
- Conclusions
- Acknowledgements
- Footnote
- References
- Jayne DG, Guillou PJ, Thorpe H, et al. Randomized trial of laparoscopic-assisted resection of colorectal carcinoma: 3-year results of the UK MRC CLASICC Trial Group. J Clin Oncol 2007;25:3061-8. [Crossref] [PubMed]
- deSouza AL, Prasad LM, Marecik SJ, et al. Total mesorectal excision for rectal cancer: the potential advantage of robotic assistance. Dis Colon Rectum 2010;53:1611-7. [Crossref] [PubMed]
- Tsujinaka S, Konishi F, Kawamura YJ, et al. Visceral obesity predicts surgical outcomes after laparoscopic colectomy for sigmoid colon cancer. Dis Colon Rectum 2008;51:1757-65; discussion 1765-7.
- Skala K, Gervaz P, Buchs N, et al. Risk factors for mortality-morbidity after emergency-urgent colorectal surgery. Int J Colorectal Dis 2009;24:311-6. [Crossref] [PubMed]
- Hellan M, Anderson C, Ellenhorn JD, et al. Short-term outcomes after robotic-assisted total mesorectal excision for rectal cancer. Ann Surg Oncol 2007;14:3168-73. [Crossref] [PubMed]
- Alsabhan F, Eftaiha S, Marecik SJ, et al. Video demonstrates our technique of combining multiple surgical modalities. Asvide 2016;3:197. Available online: http://www.asvide.com/articles/953
Cite this article as: Alsabhan F, Eftaiha S, Pai A, Prasad LM, Park JJ, Marecik SJ. Combining all forces: abdominoperineal resection in an obese male. J Vis Surg 2016;2:83.